Effect of Internet Interventions for Depression and Alcohol Use
Info: 7752 words (31 pages) Dissertation
Published: 18th Feb 2022
Tagged: HealthMental Health
Does providing a brief Internet intervention for hazardous alcohol use to people seeking online help for depression reduce both alcohol use and depression symptoms among participants with these dual disorders? Randomized controlled trial.
ABSTRACT
Background: Hazardous alcohol consumption is common among people suffering from depression. Further, there is evidence that excessive alcohol consumption among this group can make their depression worse. While many people with these dual disorders do not seek face-to-face treatment, they do seek help online. There are effective Internet interventions that target hazardous alcohol consumption or depression separately but none that combine these online interventions without the involvement of a therapist. In order to fully optimize the potential of Internet interventions, we need to develop an evidence base supporting the efficacy of Internet interventions for combined depression and hazardous alcohol use without any therapist involvement. This will allow us to capitalize on the strengths of Internet interventions – 24-hour access, wide availability and cost efficient delivery of health services. This study aims to evaluate the effects of combining an Internet intervention targeting hazardous alcohol consumption with one for depression on drinking and depressive symptoms.
Methods: A double blinded, parallel group randomized controlled trial will be used. Hazardous alcohol consumers with current depression (N=986) will be recruited from recent registrants to MoodGYM – the most widely evaluated Internet intervention for depression. Participants will be assigned, by chance, to receive just MoodGYM or to receive MoodGYM plus an extensively evaluated brief Internet intervention for hazardous alcohol consumption – Check Your Drinking. Participants will be contacted 3- and 6-months after receiving the interventions to assess changes in drinking and depression status. It is predicted that participants receiving the Check Your Drinking intervention in addition to MoodGYM will reduce their alcohol consumption to a greater extent than those who just received MoodGYM. Further predictions include the impact of receiving Check Your Drinking on improvements in depressive symptoms.
Discussion: This research will yield the crucial first steps in developing lower-cost and efficacious Internet interventions for people suffering from depression who also drink in a hazardous fashion – promoting the widespread availability of care for those in need.
KEYWORDS: clinical trial, randomized controlled trial, brief intervention, internet intervention, trial protocol, depression, hazardous alcohol use, problem drinking, comorbidity
BACKGROUND
Depression and hazardous use of alcohol contribute first and fifth to the global burden of disease in middle to high-income countries [1, 2]. Comorbidity between depression and hazardous alcohol use is common [3]. Compared to those with a single condition, such comorbid disorders are associated with persistence of symptoms, poorer treatment outcomes, and poorer social and general functioning [4, 5]. Importantly, there is emerging evidence indicating that people with comorbid depression and hazardous alcohol use will access care for their depression up to eight years sooner than they will for their alcohol concerns, providing a unique opportunity to provide early interventions for hazardous alcohol consumption [6]. Efficacious treatments for comorbid depression and hazardous alcohol use have been developed in face-to-face settings and shown to be superior to single-focused treatments [7]. However, there is a considerable gap between the need for treatment and availability of and access to effective treatment [8]. Furthermore, the majority of people with depression and hazardous alcohol use do not access treatment services [9]. The increasing availability of technology as a supplement to health care could be a potential solution to address these challenges. Internet interventions could improve both access and acceptability of treatments for these co-existing conditions and allow for broad dissemination [10-12]. In addition, delivery of the intervention online is cost-effective and can be offered flexibly in terms of time and location [12-14].
To-date, only a few randomized controlled trials have examined computer-based psychological treatment for depression and comorbid alcohol misuse; however, with promising results. Kay-Lambkin and colleagues [15] compared therapist- and computer plus therapist-delivered treatment with a single session control condition. At 12-month follow-up, both treatment options yielded superior outcomes, while computer plus therapist-based treatment showed the largest effect. A similar study compared therapist-delivered cognitive behavioral therapy and motivational interviewing, clinician-assisted computerized cognitive behavioral therapy/motivational interviewing and supportive counseling [16]. After three months, therapist-delivered and clinician-assisted computerized cognitive behavioral therapy/motivational interviewing produced superior outcomes in depression and alcohol/cannabis use compared to supportive counseling. Furthermore, change in depression levels were predicted by change in alcohol consumption. Two other trials of combined alcohol and depression Internet interventions have been conducted with youth, one finding a short-term improvement in both depression and alcohol at 3-months [17], and the other finding no impact of a personalized feedback intervention at 1-month follow-up [18].
None of these Internet-based interventions targeting adults with depression and hazardous alcohol use were conducted without the involvement of a therapist. Further, the two studies targeting youth had mixed results, small sample sizes, and only preliminary findings at a 3-month follow-up. Internet interventions without therapist involvement have the advantages of being scalable, available to those who cannot or will not access a therapist, and are accessible 24-hours a day. Given the potential advantages of such Internet interventions, it is crucial to conduct trials that address this significant gap in the literature. This study will be the first step in the development of such programs by examining the impact of combining two of the most widely evaluated and empirically supported Internet interventions for depression (MoodGYM) and drinking (Check Your Drinking).
Drinking to cope motives
While one important rationale for addressing hazardous alcohol consumption among those with depression is that providing tools to reduce alcohol consumption may reduce depressive symptoms, this study will also explore the degree to which receiving the CYD intervention and improvements in depressive symptoms are moderated by participants’ motivation to drink alcohol as a means to cope with depressive symptoms. People who drink in a hazardous manner are more likely to endorse the motivation of drinking to cope if they experience current depression compared to those who do not experience current depression [19, 20]. Unfortunately, drinking in order to counter depressive symptoms is counterproductive and can increase the severity of depressive symptoms [21-24]. This is because depression and hazardous alcohol consumption may be more functionally connected among those who drink to cope, resulting in a greater improvement in depressive symptoms among those who drink to cope with depression (as opposed to those who do not drink to cope) and who then reduce their alcohol consumption. It should be noted that the reverse may also be true – when they reduce their alcohol consumption, those with strong drinking to cope motives may in fact experience less improvement in their depressive symptoms than those with lower drinking to cope motives. However, we judge this to be less likely, given the extant literature finding that reductions in alcohol use can lead to reductions in depression [25, 26]. Nevertheless, examining whether and how drinking to cope may moderate the association between reductions in alcohol consumption and improvements in depressive symptoms is essential in order to identify mechanisms of change that will allow us to better target interventions in this vulnerable population.
Sex as a moderator of impact
Sex is another factor that may moderate the effects of the interventions on depressive symptoms and hazardous alcohol use. Incidence of depression is higher among females than among males [27]. However, males who experience depression appear more likely than females to employ externalizing behaviours, such as alcohol consumption, as a means of distracting themselves from their symptoms [28]. Previous research has demonstrated that sex and depression moderate responses to brief interventions for alcohol [29]. Specifically for women, those with higher levels of depression were less likely to respond to a brief intervention and reduce their alcohol consumption compared to women with lower levels of depression. The reverse was true for men – those with higher levels of depression were more likely to respond to a brief intervention for alcohol by reducing their alcohol consumption compared to men with lower levels of depression. Thus, examining this moderating effect will be important aspect of this study.
Aim of the study
This study will examine the impact of combining two of the most widely evaluated and empirically supported Internet interventions for depression (MoodGYM) and drinking (Check Your Drinking). Comparison of an intervention group which will be offered both MoodGYM and Check Your Drinking (CYD) to a group that receives only MoodGYM will determine whether or not the combination of online interventions is an effective way of reducing drinking and improving depressive symptoms. The primary hypotheses are:
Hypothesis 1: It is predicted that participants with co-occurring depression and problem drinking will display significant reductions in drinking behaviour in the 3- and 6-months after being provided access to the online CYD as compared to participants only provided with MoodGYM.
Hypothesis 2: Participants will co-occurring depression and problem drinking will display significant improvements in depressive symptoms in the 3- and 6-months after being provided access to the online CYD and MoodGYM intervention compared to the control group who only receive MoodGYM.
Mediational Hypothesis 3: While controlling for baseline outcomes, drinking at 3-month follow-up will change as a mediator of CYD intervention effects on depressive symptoms at 6-month follow-up.
Moderator Hypotheses 4: Participants who receive the CYD intervention and experience improvements in depressive symptoms at 3-months and 6-months will be moderated by the participants’ motivation to drink alcohol as a means to cope with depressive symptoms. It is predicted that participants who drink to cope and who then reduce their alcohol consumption will have greater improvement in depressive symptoms as opposed to those who do not drink to cope.
Moderator Hypotheses 5: Sex will moderate the impact of the Check Your Drinking (CYD) Internet intervention in predicting changes in drinking at 3- and 6-months, such that males with higher levels of depressive symptoms at baseline will demonstrate greater reductions in their alcohol consumption at follow-up compared to males with lower levels of depressive symptoms. For females, those with lower levels of depressive symptoms at baseline will be more likely to reduce their alcohol consumption after receiving the CYD compared to females who have higher levels of depressive symptoms at baseline.
METHODS/DESIGN
Participants
Online media advertising strategies from previous research studies found to be successful recruiting people with current depressive symptomatology will be used (e.g. social media ads on Facebook, and website ads on Yahoo and Google Adwords). The advertisements, placed across Canada, will target people who are ‘experiencing persistent low mood or depression’ and who are interested in participating in a study to, ‘help improve an online intervention for depression.’ All potential participants, 18 years and older, will undergo an assessment of current depression status, as well as, one to determine whether they are hazardous drinkers. Participants who score 16 or more on the Centre for Epidemiological Studies Depression scale (CES-D) [30], indicating current depression, will be eligible. In addition, participants will meet criteria for hazardous alcohol use, as indicated by a score of 8 or more on the Alcohol Use Disorder Identification Test (AUDIT) [31, 32]. Finally, in order to assess current suicidal ideation, participants will be administered the Patient Health Questionnaire (PHQ-9) [33]. All participants who are found not eligible for the study will be provided access to MoodGYM for the duration of the study.
Study Design and Procedures
This study is a two-arm, double blinded, parallel group randomized control trial of a combination of online interventions for problem drinking and depressive symptoms. Follow-ups will be conducted at 3- and 6-months. See Figure 1 for a Consort diagram of the study design.
Figure 1: Overview of the proposed intervention trial
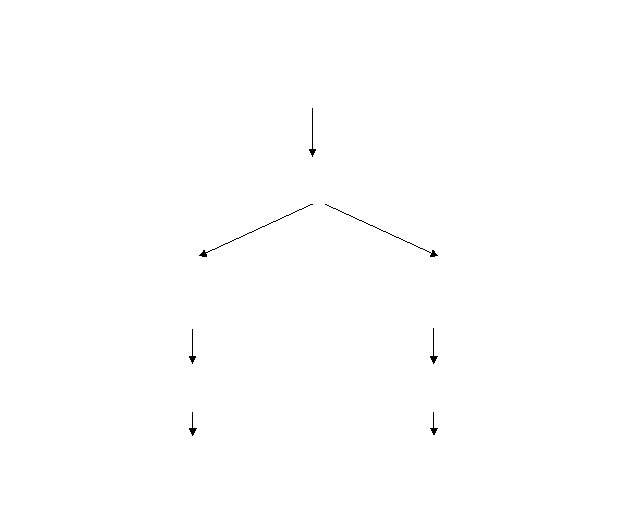
Potential participants responding to the advertisement by clicking on a link to the study website will first be provided with a brief description of the study and complete an eligibility screener (those not interested will be provided access to MoodGYM for the duration of the study). Those found eligible will be asked to provide their email address for ongoing contact as part of the study, as well as, their telephone number and mailing address as a precaution should email correspondence be unsuccessful. Participants will then be sent an email containing a consent form to be completed and returned by email. The electronic consent form will be sent in the form of a fillable pdf and word document to facilitate ease in completing the form. Those who return the completed consent form will be sent a link to complete the baseline questionnaire and be randomized into one of the two conditions. Randomization will occur via an automated replicable algorithm and to ensure a random distribution the sample will be stratified on prognostic indicators at baseline. Beyond choosing age and participants’ sex as the primary demographic variables by which to stratify, severity of current depression, severity of alcohol use (the AUDIT), and prior use of treatment for depression or for hazardous alcohol use will be employed for stratification. To reduce attrition in the study, those who complete the baseline questionnaire and access the online intervention will receive a $10 Amazon.ca gift card. All participants will be followed-up at 3- and 6-months post-randomization using an online survey (notification sent as a link to the person’s email address provided). In order to promote retention, participants completing the 3-month follow-up will be sent a $20 gift certificate from Amazon.ca and those completing the 6-month follow-up will be sent an additional $30 gift certificate from Amazon.ca (i.e. total honorarium of $60 total for each participant).
Participants who do not respond to their initial prompt to complete the follow-up surveys will be sent email reminders. All participants will then be sent three reminder emails in the next two months to log-in to the website and try a different part of the program. For participants assigned to the Intervention condition, the email reminders will also ask them to review the content of the CYD Final Report (the request to review the CYD Final Report will be removed from the reminder email once the participant has accessed this information on the MoodGYM dashboard).
Ethics approval
The research methods to be used in this study have been approved by the standing ethics review committee of the Centre for Addiction and Mental Health.
Interventions
MoodGYM only
Those randomized to this condition will be provided with access to MoodGYM but will not receive the Check Your Drinking (CYD) Final Report. MoodGYM is a popular, automated, self-help cognitive behavioral therapy program for depression comprising five modules to be completed over five weeks and an online workbook incorporating 29 exercises. MoodGYM Mark 3 has over 800,000 registrants. A series of published research trials has shown MoodGYM to be effective in reducing depressive symptoms in users in a range of settings (e.g., schools, universities, Lifeline suicide prevention, U.K. NHS Choices online), for different aspects of the mental health service spectrum (e.g., prevention vs treatment), and different age groups (adults, adolescents) [34-44]. The current trial will employ the latest version of MoodGYM (Mark 4) which has been updated to support mobile devices. The core design and function of the program has not been altered.
MoodGYM plus CYD
Those assigned to this condition will immediately be provided with access to MoodGYM and feedback from the CYD intervention will be provided as part of their MoodGYM dashboard in the form of a Final Report (items used to generate the CYD will be assessed as part of the baseline screening process). The CYD interventionis a brief and personalized online intervention that has been designed to assess and provide feedback on quantity and frequency of drinking, and severity of hazardous drinking [45]. Following the completion of an 18 item screener, the user is provided with a Final Report that compares the person’s drinking with others in the general population of the same age, sex and country of origin (Canada, the U.S.A., or the U.K.). The Final Report also includes other relevant feedback, including an assessment of severity of alcohol use, and provides recommendations for safe levels of alcohol consumption. The CYD has been subjected to five randomized trials from two independent research groups, all of which displayed a significant impact of the CYD to reduce hazardous alcohol consumption compared to controls [45-49]. The controlled access version of the CYD used in this study will be modified to include a brief description of the importance of addressing hazardous drinking among people experiencing depression prior to the intervention content.
Measures
Baseline survey
All outcome variables will ask participants about the past three months at both baseline and the corresponding follow-ups. The baseline survey will assess a series of demographic characteristics including age, participants’ sex, education, employment status, marital status, and family income. The survey will also include measures of Health related Quality of Life (HRQOL) using the WHOQoL-8. This short form version has been used in many countries, is robust psychometrically, and performance is strongly correlated with scores from the original WHOQoL [50]. Prior treatment utilization for alcohol or depression will be measured with a series of questions about past use of different treatment modalities, which have been employed in our previous research trials [37, 45], however prior and concurrent treatment accesswill not be used as inclusion/exclusion criterion (including the possibility of accessing Internet interventions for depression or alcohol).
Alcohol related measures
Following Neighbors et al. [51], the drinking outcome variables will comprise: number of drinks in a typical week (identified as the primary outcome variable for drinking), frequency of heavy drinking, and frequency of experiencing alcohol-related harm. Specifically, alcohol consumption and severity of alcohol problems will be assessed using the Alcohol Use Disorders Identification Test [32, 52]. The AUDIT is ideal for this purpose because it is well validated and distinguishes social drinkers and those with hazardous alcohol consumption [31]. Further, a score of 8 or more on the AUDIT has clinical relevance as it is recommended that clients in clinical settings receive a brief intervention from their health professional if they score at or above this cut-off [31, 53]. Number of drinks consumed on each day in a typical week [51, 54, 55], and frequency of heavy drinking will be assessed using a composite of four items from the Alcohol Consumption Index [56]. Alcohol-related problems will be assessed using the Rutgers Alcohol Problem Index (RAPI) [57], modified to apply to an adult population. Individuals in the intervention condition will be asked the five-item coping subscale of the Drinking Motives Questionnaire [58] and several other items at baseline in order to generate the CYD Final Report – usual amount paid for a drink; weight (to generate time under the influence of alcohol); and whether alcohol had a harmful effect on respondents’ (i) friendships/social life, (ii) physical health, (iii) outlook on life (happiness), (iv) home life or marriage, (v) work, studies, or employment opportunities, or (vi) financial position [59].
Mental Health
Depressive symptoms will be assessed using the 20-item Centre for Epidemiological Studies Depression scale (CES-D) [30]. In addition, the PHQ-9 questionnaire will be employed to identify participants with suicidal ideation [33]. Anxiety symptoms will be assessed using the GAD-7 [60].
Follow-up Surveys
All participants will be followed-up at 3 and 6 months’ time and asked about their current depressive symptomatology, as well as, their alcohol consumption in the time since their last assessment. All items in the follow-ups will ask about the last three months. Both surveys will assess:
(1) Drinking and alcohol-related harm using the same outcome variables used at baseline;
(2) Current depressive and anxiety symptoms using the CES-D, the PHQ-9 and the GAD-7;
(3) Health related Quality of Life (HRQOL) using the WHOQoL-8;
(4) Formal addictions treatment utilization will be measured using the same items as the baseline survey.
Use of Interventions
The amount and type of use participants make of the MoodGYM intervention (as well as the number of times the CYD Final Report is viewed) will be recorded and this information will be used in secondary analyses to test whether degree of involvement is related to reductions in drinking and depressive symptoms. Following methods used by Danaher (2008) and Strecher (2008), we will operationalize degree of involvement with MoodGYM by recording the number of times the participant accesses the site, as well as, the number of tools the participant uses (as assessed by page views, form completions, etc.) and length of involvement with the site (e.g. use of the site over time) [61, 62].
Power Analysis
Power calculations were conducted using the G-power software application [63]. Estimates provided by G-power are based on conventions established by Jacob Cohen’s work on power analysis [64, 65]. Based on previous evaluations of CYD and similar web-based brief alcohol interventions [66], we expect effects on drinking to be in the small range (e.g., Cohen, 1992; d =.20). We expect small to moderate effect sizes in associations between drinking and depressive symptoms. Moreover, we estimated sample size based on ability to detect small univariate effects on drinking and depression outcomes, as well as, considering the need to have sufficient males and females to conduct the proposed analysis of the moderating role of sex on the impact of the CYD (approximately 70% of the sample will be female based on previous research employing similar recruitment strategies) [67]. Given maximum expected attrition, a sample size of 788 will provide .80 power to detect effects sizes of d = .20. We anticipate adequate power to detect effects throughout the anticipated range.
Based on our previous work, we expect a retention rate of 80% across both 3- and 6-month follow-ups [45]. Thus, we will recruit an initial sample of 986 participants. We anticipate needing approximately 6,000 responses to our recruitment advertisement. Of these, roughly 2,000 will be eligible for the trial as approximately one-third of potential participants responding to the initial recruitment advertisement will be hazardous alcohol consumers [68]. Based on our prior experience, about half of these will actually consent and be randomized to condition (N = 986).
Data Analysis
All analyses will be undertaken on an intention-to-treat basis using all available data as suggested by White et al. [69]. Hypotheses will be tested using a generalized linear hypothesis framework [70]. This analytic approach allows the sophisticated handling of missing data using multiple imputations. Hypothesis 1 and 2 will evaluate main effects of CYD on drinking and depressive symptoms respectively. With respect to evaluating main effects of experimental conditions on drinking, each participant will provide baseline, 3-month, and 6-month follow-up data. Baseline differences in demographics will be included as covariates to address any potential differences. A dummy-coded contrast will represent the Intervention versus Control condition. Distributions of outcome variables are likely to be non-normal (e.g., negative binomial) and we will adjust the analysis to utilize an appropriate distribution, as we have done in previous work [51, 71]. Analyses will examine specific effects on 3- and 6-month outcomes to provide precise evaluation of the duration of effects. However, we will also conduct longitudinal analyses to provide a comprehensive examination of changes over the course of the trial. Longitudinal analyses will utilize a generalized linear mixed modeling approach, where distributions of outcomes are considered and appropriately specified and random effects are used to account for nesting of assessment points within individuals (see Atkins et al., 2013 for descriptions of this approach). An alternative GEE approach will be used in the event of convergence problems which often arise in specification of random effects for zero-inflated distributions.
Hypothesis 3 will evaluate changes in drinking at 3-month follow-up as a mediator of CYD intervention effects on depressive symptoms at 6-month follow-up. We will follow procedures described by MacKinnon and colleagues [72] to assess mediation. Mediation will test indirect effects using the AB products method where A will represent effects of intervention on 3-month drinking. B will represent the associations of 3-months drinking on 6-months depressive symptoms. Both A and B paths will control for baseline outcomes. We will use bootstrapping to obtain standard errors for the indirect (AB) pathway, which accounts for the asymmetric distribution of standard errors of products [73].
Moderator Hypotheses 4 and 5 will extend the main effects models and will include relevant product terms. Hypothesis 5 represents a three-way interaction between participants’ sex, intervention condition, and baseline depressive symptoms in predicting changes in drinking at 3- and 6-months. Predictors will include the three-way product terms, constituent two-way product terms, and main effects. While the three-way interaction is our primary prediction here, we will also examine constituent two-way interactions. All significant interactions will be graphed and accompanied by tests of simple slopes using procedures described by Cohen and colleagues [74]. Moderator Hypothesis 4 will be evaluated using the same approach where depressive symptoms at 3- and 6-months will be evaluated as a function of the intervention condition, baseline coping motives, and the intervention by coping motives product term.
Finally, secondary analyses not described here will investigate any impact of the interventions on health related quality or life and test the extent to which degree of involvement with the Internet interventions are related to outcome.
DISCUSSION
The majority of people with depression and hazardous alcohol use do not access treatment services [9]. There is also a considerable gap between the need and availability of treatment and access to effective treatment [8]. The increasing availability of technology as a supplement to health care could be a potential solution to address these challenges. In addition, these Internet interventions conducted without therapist involvement have the advantages of being scalable, available to those who cannot or will not access a therapist, and are accessible 24-hours a day. Given the potential advantages of such Internet interventions, it is crucial to conduct trials that address this significant gap in the literature. This study will be the first step in the development of such programs by examining the impact of combining two of the most widely evaluated and empirically supported Internet interventions for depression (MoodGYM) and for drinking (Check Your Drinking). The brief nature of the CYD and the substantial research base indicating the efficacy of the CYD among people who consume alcohol in a hazardous fashion suggest the next natural step of research on this topic is to explore the extent to which the CYD can be applied among vulnerable populations, such as those with depression. In addition, the results of this study will enhance our general understanding of Internet interventions for addictions, as well as inform how treatments can be developed and matched to the care of need for those with co-occurring mental health and drinking issues.
List of abbreviations
CYD – Check Your Drinking
CES-D – Centre for Epidemiological Studies Depression scale
AUDIT – Alcohol Use Disorder Identification Test
PHQ-9 – Patient Health Questionnaire 9 item scale
HRQOL – Health Related Quality of Life
WHOQoL-8 – World Health Organization Quality of Life
RAPI – Rutgers Alcohol Problem Index
GAD-7 – Generalized Anxiety Disorder 7 item scale
References
1. The global burden of disease: 2004 update [http://www.who.int/healthinfo/global_burden_disease/2004_report_update/en/]
2. Whiteford HA, Degenhardt L, Rehm J, Baxter AJ, Ferrari AJ, Erskine HE, Charlson FJ, Norman RE, Flaxman AD, Johns N et al: Global burden of disease attributable to mental and substance use disorders: findings from the Global Burden of Disease Study 2010. Lancet 2013, 382:1575-1586.
3. Bolton JM, Robinson J, Sareen J: Self-medication of mood disorders with alcohol and drugs in the National Epidemiologic Survey on Alcohol and Related Conditions. J Affect Disord 2009, 115(3):367-375.
4. Quello SB, Brady KT, Sonne SC: Mood disorders and substance use disorder: a complex comorbidity. Science & practice perspectives / a publication of the National Institute on Drug Abuse, National Institutes of Health 2005, 3(1):13-21.
5. Davis LL, Frazier E, Husain MM, Warden D, Trivedi M, Fava M, Cassano P, McGrath PJ, Balasubramani GK, Wisniewski SR et al: Substance Use Disorder Comorbidity in Major Depressive Disorder: A Confirmatory Analysis of the STAR*D Cohort. Amer J Addict 2006, 15(4):278-285.
6. Kay-Lambkin FJ: Lifetime affective and alcohol use disorders: impact of comorbidity on current functioning and service use in a rural population. J Addict Res Ther 2014, S10:009.
7. Baker AL, Kavanagh DJ, Kay-Lambkin FJ, Hunt SA, Lewin TJ, Carr VJ, Connolly J: Randomized controlled trial of cognitive–behavioural therapy for coexisting depression and alcohol problems: short-term outcome. Addiction 2010, 105(1):87-99.
8. Kohn R, Saxena S, Levav I, Saraceno B: The treatment gap in mental health care. Bulletin of the World Health Organization 2004, 82(11):858-866.
9. Clarkin JF, Kendall PC: Comorbidity and treatment planning: summary and future directions. J Consult Clin Psychol 1992, 60(6):904-908.
10. Kaltenthaler E, Parry G, Beverley C, Ferriter M: Computerised cognitive-behavioural therapy for depression: systematic review. Br J Psychiatry 2008, 193(3):181-184.
11. Cuijpers P, van Straten A, Andersson G: Internet-administered cognitive behavior therapy for health problems: a systematic review. J Behav Med 2008, 31(2):169-177.
12. Bewick BM, Trusler K, Barkham M, Hill AJ, Cahill J, Mulhern B: The effectiveness of web-based interventions designed to decrease alcohol consumption – A systematic review. Prev Med 2008, 47(1):17-26.
13. Cunningham JA, Humphreys K, Koski-Jannes A: Providing personalized assessment feedback for problem drinking on the Internet: a pilot project. J Stud Alcohol 2000, 61(6):794-798.
14. Cunningham JA, Kypri K, McCambridge J: The use of emerging technologies in alcohol treatment. Alcohol Res Health 2011, 33(4):320-326.
15. Kay-Lambkin FJ, Baker AL, Lewin TJ, Carr VJ: Computer-based psychological treatment for comorbid depression and problematic alcohol and/or cannabis use: a randomized controlled trial of clinical efficacy. Addiction 2009, 104(3):378-388.
16. Kay-Lambkin FJ, Baker AL, Kelly B, Lewin TJ: Clinician-assisted computerised versus therapist-delivered treatment for depressive and addictive disorders: a randomised controlled trial. Med J Australia 2011, 195(3):S44-50.
17. Deady M, Mills KL, Teesson M, Kay-Lambkin FJ: A randomised controlled trial of an online intervention for co-occurring depression and problematic alcohol use in young people: Primary outcomes. J Med Internet Res 2016, 18:e71.
18. Geisner IM, Varvil-Weld L, Mittmann AJ, Mallett K, Turrisi R: Brief web-based intervention for college students with comorbid risky alcohol use and depressed mood: Does it work and for whom? Addict Behav 2015, 42:36-43.
19. Nolen-Hoeksema S, Desrosiers A, Wilsnack SC: Predictors of alcohol-related problems among depressed and non-depressed women. J Affect Disord 2013, 150(3):967-973.
20. Foster DW, Young CM, Steers MN, Quist MC, Bryan JL, Neighbors C: Tears in your beer: Gender differences in coping drinking motives, depressive symptoms and drinking. Int J Ment Health Addiction 2014, 12:730-746.
21. Aneshensel CS, Huba GJ: Depression, Alcohol-Use, and Smoking over One Year – a 4-Wave Longitudinal Causal Model. J Abnorm Psychol 1983, 92(2):134-150.
22. Hartka E, Johnstone B, Leino EV, Motoyoshi M, Temple MT, Fillmore KM: A Metaanalysis of Depressive Symptomatology and Alcohol-Consumption over Time. Brit J Addict 1991, 86(10):1283-1298.
23. Kwon TY, Kahng SK, Kim H: The reciprocal relationship between depressive symptoms and alcohol consumption: Group comparison by employment status. Asian Soc Work Pol Rev 2010, 4:43-56.
24. Holahan CJ, Moos RH, Holahan CK, Cronkite RC, Randall PK: Drinking to cope and alcohol use and abuse in unipolar depression: A 10-year model. J Abnorm Psychol 2003, 112(1):159-165.
25. Brown SA, Schuckit MA: Changes in Depression among Abstinent Alcoholics. J Stud Alcohol 1988, 49(5):412-417.
26. Davidson KM: Diagnosis of Depression in Alcohol Dependence – Changes in Prevalence with Drinking Status. Br J Psychiatry 1995, 166:199-204.
27. Kessler RC, Mcgonagle KA, Swartz M, Blazer DG, Nelson CB: Sex and Depression in the National Comorbidity Survey .1. Lifetime Prevalence, Chronicity and Recurrence. J Affect Disord 1993, 29(2-3):85-96.
28. Nolen-Hoeksema S: Gender differences in depression. In: Handbook of depression. edn. Edited by Hammen IHGCL. New York: Guilford Press; 2002: 492-509.
29. Merrill JE, Reid AE, Carey MP, Carey KB: Gender and Depression Moderate Response to Brief Motivational Intervention for Alcohol Misuse Among College Students. Journal of Consulting and Clinial Psychology 2014, 82:984-992.
30. Radloff LS: The CES-D scale: A self report depression scale for research in the general population. Applied Psychol Meas 1977, 1:385-401.
31. Saunders JB, Aasland OG, Babor TF, De La Fuente JR, Grant M: Development of the Alcohol Use Disorders Identification Test (AUDIT): WHO collaborative project on early detection of persons with harmful alcohol consumption— II. Addiction 1993, 88:791-804.
32. Babor TF, De La Fuente MF, Saunders JB, Grant M: AUDIT – The alcohol use disorders identification test: Guidelines for use in primary health care. Geneva, Switzerland: World Health Organization; 1989.
33. Kroenke K, Spitzer RL, Williams JBW: The PHQ-9 – Validity of a brief depression severity measure. J Gen Intern Med 2001, 16(9):606-613.
34. Bennett K, Reynolds J, Christensen H, Griffiths KM: e-hub: an online self-help mental health service in the community. Med J Australia 2010, 192(11):S48-S52.
35. Calear AL, Christensen H, Mackinnon A, Griffiths KM, O’Kearney R: The YouthMood Project: A Cluster Randomized Controlled Trial of an Online Cognitive Behavioral Program With Adolescents. J Consult Clin Psychol 2009, 77(6):1021-1032.
36. Christensen H, Griffiths KM, Jorm AF: Delivering interventions for depression by using the internet: randomised controlled trial. Brit Med J 2004, 328(7434):265-268A.
37. Griffiths KM, Christensen H, Jorm AF, Evans K, Groves C: Effect of web-based depression literacy and cognitive-behavioural therapy interventions on stigmatising attitudes to depression – Randomised controlled trial. Br J Psychiatry 2004, 185:342-349.
38. Hickie IB, Davenport TA, Luscombe GM, Moore M, Griffiths KM, Christensen H: Practitioner-supported delivery of internet-based cognitive behaviour therapy: evaluation of the feasibility of conducting a cluster randomised trial. Med J Australia 2010, 192(11):S31-S35.
39. Hoifodt RS, Lillevoll KR, Griffiths KM, Wilsgaard T, Eisemann M, Waterloo K, Kolstrup N: The Clinical Effectiveness of Web-Based Cognitive Behavioral Therapy With Face-to-Face Therapist Support for Depressed Primary Care Patients: Randomized Controlled Trial. J Med Internet Res 2013, 15(8).
40. Mackinnon A, Griffiths KM, Christensen H: Comparative randomised trial of online cognitive-behavioural therapy and an information website for depression: 12-month outcomes. Br J Psychiatry 2008, 192(2):130-134.
41. O’Kearney R, Kang K, Christensen H, Griffiths K: A Controlled Trial of a School-Based Internet Program for Reducing Depressive Symptoms in Adolescent Girls. Depress Anxiety 2009, 26(1):65-72.
42. Phillips R, Schneider J, Molosankwe I, Leese M, Foroushani PS, Grime P, McCrone P, Morriss R, Thornicroft G: Randomized controlled trial of computerized cognitive behavioural therapy for depressive symptoms: effectiveness and costs of a workplace intervention. Psychol Med 2014, 44(4):741-752.
43. Powell J, Hamborg T, Stallard N, Burls A, McSorley J, Bennett K, Griffiths KM, Christensen H: Effectiveness of a Web-Based Cognitive-Behavioral Tool to Improve Mental Well-Being in the General Population: Randomized Controlled Trial. J Med Internet Res 2013, 15(1):2-18.
44. Sethi S: Treating Youth Depression and Anxiety: A Randomised Controlled Trial Examining the Efficacy of Computerised versus Face-to-face Cognitive Behaviour Therapy. Aust Psychol 2013, 48(4):249-257.
45. Cunningham JA, Wild TC, Cordingley J, van Mierlo T, Humphreys K: A randomized controlled trial of an internet-based intervention for alcohol abusers. Addiction 2009, 104(12):2023-2032.
46. Doumas DM, Hannah E: Preventing high-risk drinking in youth in the workplace: A web-based normative feedback program. J Subst Abuse Treat 2008, 34(3):263-271.
47. Doumas DM, Haustveit T: Reducing heavy drinking in intercollegiate athletes: Evaluation of a web-based personalized feedback program. The Sport Psychologist 2008, 22:213-229.
48. Doumas DM, McKinley LL, Book P: Evaluation of two Web-based alcohol interventions for mandated college students. J Subst Abuse Treat 2009, 36(1):65-74.
49. Cunningham JA, Murphy M, Hendershot CS: Treatment dismantling pilot study to identify the active ingredients in personalized feedback interventions for hazardous alcohol use: Randomized controlled trial. Addict Sci Clin Pract 2014, e9:22.
50. Schmidt S, Muhlan H, Power M: The EUROHIS-QOL 8-item index: psychometric results of a cross-cultural field study. Eur J Public Health 2006, 16(4):420-428.
51. Neighbors C, Lewis MA, Atkins DC, Jensen MM, Walter T, Fossos N, Lee CM, Larimer ME: Efficacy of Web-Based Personalized Normative Feedback: A Two-Year Randomized Controlled Trial. J Consult Clin Psychol 2010, 78(6):898-911.
52. Saunders JB, Conigrave KM: Early identification of alcohol problems. Cmaj 1990, 143:1060-1069.
53. National Institute on Alcohol Abuse and Alcoholism: Helping patients who drink too much: A clinician’s guide. Rockville, MD: National Institute on Alcohol Abuse and Alcoholism; 2005.
54. Romelsjö A, Leifman H, Nyström S: A comparative study of two methods for the measurement of alcohol consumption in the general population. Int J Epidemiol 1995, 24:929-936.
55. Kühlhorn E, Leifman H: Alcohol surveys with high and low coverage rate: A comparative analysis of survey strategies in the alcohol field. J Stud Alcohol 1993, 54:542-544.
56. Knee CR, Neighbors C: Self-determination, perception of peer pressure, and drinking among college students. J Appl Soc Psychol 2002, 32(3):522-543.
57. White HR, Labouvie EW: Towards the Assessment of Adolescent Problem Drinking. J Stud Alcohol 1989, 50(1):30-37.
58. Cooper ML: Motivations for alcohol use among adolescents: Development and validation of a four-factor model. Psychol Assess 1994, 6:117-128.
59. Bondy SJ, Lange P: Measuring alcohol-related harm: Test-retest reliability of a popular measure. Subst Use Misuse 2000, 35:1263-1275.
60. Spitzer RL, Kroenke K, Williams JBW, Lowe B: A brief measure for assessing generalized anxiety disorder – The GAD-7. Arch Intern Med 2006, 166(10):1092-1097.
61. Danaher BG, Smolkowski K, Seeley JR, Severson HH: Mediators of a successful web-based smokeless tobacco cessation program. Addiction 2008, 103(10):1706-1712.
62. Strecher VJ, McClure J, Alexander G, Chakraborty B, Nair V, Konkel J, Greene S, Couper M, Carlier C, Wiese C et al: The role of engagement in a tailored web-based smoking cessation program: randomized controlled trial. J Med Internet Res 2008, 10(5):e36.
63. Faul F, Erdfelder E, Lang AG, Buchner A: G*Power 3: a flexible statistical power analysis program for the social, behavioral, and biomedical sciences. Behav Res Methods 2007, 39(2):175-191.
64. Cohen J: A power primer. Psychological Bulletin 1992, 112:155-159.
65. Cohen J: Statistical power analysis for the behavioral sciences. Hillsdale, N.J: Lawrence Erlbaum Associates; 1988.
66. Riper H, Blankers M, Hadiwijaya H, Cunningham J, Clarke S, Wiers R, Ebert D, Cuijpers P: Effectiveness of guided and unguided low-intensity internet interventions for adult alcohol misuse: a meta-analysis. PloS one 2014, 9(6):e99912.
67. Donker T, Bennett K, Bennett A, Mackinnon A, van Straten A, Cuijpers P, Christensen H, Griffiths KM: Internet-delivered interpersonal psychotherapy versus internet-delivered cognitive behavioral therapy for adults with depressive symptoms: randomized controlled noninferiority trial. J Med Internet Res 2013, 15(5):e82.
68. Farrer L, Christensen H, Griffiths KM, Mackinnon A: Web-based cognitive behavior therapy for depression with and without telephone tracking in a national helpline: secondary outcomes from a randomized controlled trial. J Med Internet Res 2012, 14(3):e68.
69. White IR, Horton NJ, Carpenter J, Pocock SJ: Strategy for intention to treat analysis in randomised trials with missing outcome data. Bmj 2011, 342:d40.
70. Fox J: Applied regression analysis and generalized linear models, 2nd edn. Los Angeles: Sage; 2008.
71. Atkins DC, Baldwin SA, Zheng C, Gallop RJ, Neighbors C: A Tutorial on Count Regression and Zero-Altered Count Models for Longitudinal Substance Use Data (vol 27, pg 166, 2012). Psychol Addict Behav 2013, 27(2):379-379.
72. MacKinnon DP, Fairchild AJ, Fritz MS: Mediation analysis. Annu Rev Psychol 2007, 58:593-614.
73. Hayes AF: Introduction to Mediation, Moderation, and Conditional Process Analysis: A Regression-Based Approach. New York: Guildford Press; 2013.
74. Cohen J, Cohen P, West SG, Aiken LS: Applied multiple regression/correlation analysis for the behavioral sciences, 2nd. edn: Routledge; 2013.
Cite This Work
To export a reference to this article please select a referencing stye below:
Related Services
View allRelated Content
All TagsContent relating to: "Mental Health"
Mental Health relates to the emotional and psychological state that an individual is in. Mental Health can have a positive or negative impact on our behaviour, decision-making, and actions, as well as our general health and well-being.
Related Articles
DMCA / Removal Request
If you are the original writer of this dissertation and no longer wish to have your work published on the UKDiss.com website then please:




