Nutritional Interventions to Stop Hypertension
Info: 7410 words (30 pages) Dissertation
Published: 9th Dec 2019
Abstract
The overall study of this essay is to show nutritional interventions to prevent or control hypertension. In addition, this paper shows the implications of uncontrolled hypertension. The goal is to illustrate to the reader the functional changes to the human body that occurs with hypertension. It will show the factors that influence high blood pressure, such as obesity, genetics, and unhealthy nutritional patterns. It will give definition to the different types of hypertension and the changes that need to be made to control high blood pressure. The new guideline for blood pressure measurement will also be briefly outlined. One interesting point that will be analyzed, is the role of the gastrointestinal system and how it regulates the vascular function and blood pressure. The reader will learn that more than sixty percent of the risk factors for hypertension is associated with the metabolic system.
Next, this paper will explore the building block of how proteins, carbohydrates, and fats influence the bad and the good cholesterol levels and examples of the risk factors of hypertension-related illnesses. In addition, this paper shows the effects of how vitamins and minerals play an essential part in the regulation of blood pressure. Moving on, the reader will learn the five overarching guidelines provided by the 2015-2020 Dietary Guidelines which motivate individuals to make healthier lifestyle changes. To encourage people to include better food choices at meal time the U.S Department of Agriculture produced a symbol called MyPlate. This feature is briefly discussed to show the balance of food proportion at every meal.
Another essential point that will be viewed is the evidence-based diet plans. Particular points will be the nutritional interventions such as the Dash diet and the Mediterranean diet. This will include some of the similarities between the two diets and the different features they promote. It will include some interesting facts like the Dash diet was originally developed to lower blood pressure and with some research, it has shown that the Dash diet also reduces the risk of other diseases. In addition, the Mediterranean diet has implemented foods native to the countries surrounding the Mediterranean Sea. It is known that these people have a lower risk of diseases than those of the United States. Both of these diets are highly recommended by healthcare professionals to promote a better quality of life and reduce the risk of diseases. Lastly, this essay provides a brief outline of the important role of the nurse and patient education. It will include ideas of educational materials to use that best fits the patient.
Nutritional Interventions to Stop Hypertension
Hypertension is on the rise. The lead author of the new high blood pressure guidelines, Paul K. Whelton, MB, MD, MSc, FACC notes, that the statistics show that one out of three Americans have high blood pressure. In 2017 a correction was made by the American Heart Association and the American College of Cardiology and they express that at least half of the United States are hypertensive (New ACC/AHA High Blood Pressure Guidelines). Now with the new corrections, people with a systolic blood pressure of 130 and a diastolic blood pressure of 80 are deemed of stage one hypertension. With hypertension being the leading cause of death worldwide, executing better eating patterns like the Dash diet and the Mediterranean diet urge people to incorporate an assortment of foods with an abundance of nutrients that assist in lowering blood pressure. Adjusting nutritional and other lifestyle changes are an imperative step to effectively prevent and treat high blood pressure and the chance of other cardiovascular disease.
Pathophysiology & Etiology of Hypertension
High blood pressure is the force of blood that is pushing against the wall of the blood vessels, consistently too high, which in turn makes the heart and blood vessels work less efficiently (American Heart Association, 2016). When consuming an unhealthy diet for a long period of time fats form along the wall of the arteries and eventually weakens the elasticity of the vessels which in turn affects the blood flow through the body (High Blood Pressure: Hypertension, 2016). McCance and Huether (2019) noted, “hypertension is caused by increases in cardiac output, total peripheral resistance, or both. Cardiac output is increased by any condition that increases heart rate (beats per minute) or stroke volume (millimeters of blood ejected during ventricular systole), whereas peripheral resistance is increased by any factor that increases blood viscosity or reduce vessel diameter (vasoconstriction)” (p.1061). Some individuals have isolated systolic hypertension. Isolated systolic hypertension (ISH) is elevated systolic blood pressure accompanied by normal diastolic blood pressure. ISH is becoming more widespread among both genders and is associated with cardiovascular and cerebrovascular events (McCance, K.L & Huether, S.E, 2019, p1062)
There are two classifications for hypertension, primary and secondary. Primary hypertension has no known causes. Normally individuals with primary hypertension do not require medication therapy but rather a lifestyle change such as increasing physical activity, nutritional interventions and smoking cessation. Secondary hypertension is associated with other underlying medical condition that could impact the kidneys and the heart. Appropriate treatment for this type of hypertension will most often control the underlying medical issue and high blood pressure. (McCance, K.L & Huether, S.E; 2019, p. 1138). “Numerous genetic vulnerabilities have been linked to hypertension and these, in combination with environmental risks, cause neurohumoral dysfunction (sympathetic nervous system, renin-angiotensin-aldosterone system, and natriuretic hormones) and promote inflammation and insulin resistance. Insulin resistance and neurohumoral dysfunction contribute to sustained systemic vasoconstriction and increased peripheral resistance. Inflammation contributes to renal dysfunction, which, in combination with the neurohumoral alterations, results in renal salt and water retention and increased blood volume. Increased peripheral resistance and increased blood volume are two primary causes of sustained hypertension” (McCance, K.L & Huether, S.E, 2019, p. 1062).
Symptoms and Complications of Untreated Hypertension
Hypertension is known as the silent killer because there are no symptoms to alert the individual that they have high blood pressure. Most people do not know they have high blood pressure until they get their blood pressure checked by a doctor. Hypertension is related to numerous comorbidity conditions such as irregular heartbeat, vision issues, headaches, and chest pain (CDC gov, 2018). Unfortunately, women after menopause are at a higher risk of heart attacks as a result of hormone changes. The appearances are one of a kind for women and can be effortlessly dismissed for something else, for example, heavy perspiration, stomach pain, and upper body pain like the neck, jaw and upper arms. Hypertension prompts other common cardiovascular maladies such as myocardial infarction and stroke (McCance, K.l & Huether, S.E, 2019).
Anybody can have hypertension, but the American Heart Association says African Americans are more prone to high blood pressure than white Americans and that African Americans have the highest percentage of hypertension in the world. Although the reason is still unclear, researchers are suggesting there may be an angiotensin converting enzyme (ACE) variant gene that causes African Americans to be more sensitive to salt. For those who have this gene, as little as half a teaspoon of salt, which is approximately 1000 mg of sodium or two and five tenths of a gram, can make their blood pressure elevate as much as five mmHg (American Heart Association, 2018). The major health organizations recommend individuals consume less than 1500 mg of sodium per day, which is seventy-five hundredths of a teaspoon of salt. The result of increased sodium consumption and having consistently high blood pressure without treatment can damage your arteries such as the kidneys. It is important to remember, individuals who are salt sensitive still need to adhere to preventive measures to prevent or make improvements in their hypertensive condition (American Heart Association, 2018).
Hypertension is a standout amongst the most widely recognized reasons for kidney failure. That is on the grounds that it can harm both large arteries leading to the kidneys and the small veins (glomeruli) within the kidneys. Compromise to either makes it difficult for the kidneys to filter out waste from the blood. Under those circumstances, excessive amount of fluid and waste can accumulate. This may eventually lead to needing kidney dialysis or transplantation. In result, low sodium diets are necessary to decrease hypertension and fluid build-up around the organs. (High Blood Pressure Affects Digestion).
At this point when hypertension goes untreated, serious complications can happen because organs are compromised which could lead to death. In relation, individuals with systolic blood pressure greater than 180mmHG or diastolic blood pressure greater than 120mmHg is called hypertensive emergency, and at this point end-organ damage is present. Hypertensive emergency is rare, be that as it may, manifestations incorporate blurry vision, nausea, chest pain and anxiety (High Blood Pressure Dangers: Hypertension; 2106).
Diagnosis and Treatment
It takes more than one elevated blood pressure to be diagnosed with hypertension. To get an accurate diagnosis the healthcare provider will get two or three readings on separate appointments to rule out inaccuracies such as white coat hypertension (elevated blood pressure that occurs in a clinical setting) and masked hypertension (normal blood pressure in a clinical setting but elevated elsewhere). Twenty-four-hour blood pressure monitor test or ambulatory blood pressure monitoring may also be recommended to show blood pressure changes throughout the day and night (McCance, K.L & Huether, S.E, 2019, p. 1066). This requires the individual to not smoke or consume coffee prior to the appointment for this could raise blood pressure measurements. Ambulatory measurement also detects those who fail to have a nocturnal decrease in blood pressure and who may be at a higher cardiovascular risk. It is especially recommended for individuals with drug resistance, hypotensive symptoms with medications, episodic hypertension, and autonomic dysfunction (McCance, K.L & Huether, S.E, 2019, p. 1066).
Once an individual has been diagnosed with high blood pressure the physician may suggest an electrocardiogram. This procedure checks for signs of heart disease by measuring the thickness of the heart muscle, check for poor blood flow, signs of a heart attack and heart rhythm. By doing so a technician will apply small electrode patches on the chest, arms, and legs, which then records the electrical activity of the heart (Diagnosing High Blood Pressure).
An echocardiogram may also be requested by the physician. This test uses ultrasound to evaluate the heart muscle and the heart valves. This procedure would assess the overall function of the heart, determine the presence of many types of heart disease, follow the progress of heart valve disease over time and evaluate the effectiveness of medical or surgical treatments. There are many types of echocardiograms and your physician will determine which one will benefit your needs (Diagnosing High Blood Pressure).
Digestion Absorption and Metabolism
Digestion is the process whereby food is broken down into smaller pieces. It first begins with mechanical digestion via the teeth that physically breaks down large junks of food into smaller pieces and the food is being mixed with saliva by means of chemical digestion. Chemical digestion breaks down large food particles, for example, proteins, lipids, nucleic acids, and starches must be broken down into subunits that are small enough to be absorbed by the lining of the alimentary canal. This is accomplished by enzymes through hydrolysis. Chemical digestion consists of numerous chemical reactions catalyzed by enzymes in saliva, gastric juice, pancreatic juice, and intestinal juice (Thibodeau, G. A., & Patton, K. T. 2016, p. 383). Once in the stomach it stores and churns the food. The process of intestinal digestion is initiated in the stomach by the actions of gastric hydrochloride and pepsin, which activates enzymes and breaks up the food more. The chyme that passes into the duodenum is a liquid that contains small particles of undigested food. Digestion continues in the small intestine by the action of pancreatic enzymes, intestinal brush-border enzymes and bile salts. Carbohydrates are broken down to monosaccharides and disaccharides in the proximal small intestine, proteins are degraded further into amino acids and peptides, and fats are emulsified and reduced to fatty acids and monoglycerides. After the food is digested, the resulting nutrients are absorbed and move through the mucous membrane lining of the small intestine into the blood and lymph (McCance, K. L., & Huether, S. E. 2019, p. 1301). Then the next phase is metabolism, which could be the main element of hypertension.
Metabolism is the process of the way nutrients from foods are used to energize the body and to form and maintain body structures and functions. Two processes of metabolism involve catabolism and anabolism. Catabolism is all the chemical reactions that release energy from nutrient molecules (Thibodeau, G.A.; & Patton, K.T. 2016, p.396). This is a vital process because it is the only way the body has of supplying it with energy for doing any work. Catabolism breaks nutrient molecules down into smaller molecules and releases energy called Adenosine Triphosphate (ATP) in the process. As soon as ATP is made, the many chemical reactions that build nutrient molecules into more complex chemical compounds constitute the process of anabolism (Thibodeau, G. A., & Patton, K. T. 2016, p. 396). The anabolic reaction uses ATP to produce molecules that the cell needs to keep working and stores the left over molecule for later use.
The gastrointestinal system plays an important role regulating the vascular function and blood pressure. A piece of evidence from clinical modifications show improvement of hypertension and related cardiometabolic diseases. More than sixty percent of the risk factors for hypertension are associated with metabolic disorders (Zhu, Z; Xiong, S.; & Liu, D) Some types of hypertension can be induced by metabolic disturbances and can be defined as metabolic hypertension. However, the pathogenesis of metabolic hypertension remains largely unknown. The gastrointestinal tract is a gate through which internal food, metabolites, and microbes enter the human body (Zhu, Z; Xiong, S & Liu, D) Thus, metabolism related risk factors may affect blood pressure through the gastrointestinal and alter processes such as taste perception, mucosal absorption, gut hormone homeostasis, GI nerve activity, and gut microbiota. Meanwhile, gastrointestinal intervention through dietary approaches, gut microbiota modification and metabolic surgery could profoundly improve or remit the vascular dysfunction and metabolic hypertension. Even though more studies are needed, Zhu, Xiong and Liu suggest that the gastrointestinal intestinal tract could be the initial organ of metabolic hypertension (Zhu, Z.; Xiong, S.;& Liu, D; n.d).
Another interesting aspect of how hypertension affects the digestion system is normally when we eat our body naturally shuts off the blood supply to other areas of the body to increase blood supply to your stomach and intestines, so they can perform their jobs. With high blood pressure already present, the arteries to the capillaries become damaged. This allows less blood to make it to the stomach and intestines. Without added blood, the digestive system is not able to perform at a normal level and can lead to a variety of digestion problems (High Blood Pressure Affects Digestion).
Effects of Carbohydrates, Protein and Fats
Carbohydrates, protein, and fats are the principle calorie sources in the American diet. Adjusting the calories that we take in and consume every day can help us maintain, lose or gain weight. There are two classifications of carbohydrates, carbohydrates are classified as simple and complex both of which are valuable sources of energy but provide different levels of nutrient density. Complex carbohydrates can be found in fruits, vegetables, and whole grains. Complex carbs contain fiber that helps with digestive regularity and the feeling of fullness. Food high in fiber additionally help with lowering cholesterol and decreases the risk of heart disease. Simple carbohydrates primarily provide energy in the form of glucose, fructose, galactose and have minimal nutritional value (Grodner, M.D, 2019, p.53). Other simple carbohydrates such as sodas, table sugar, and candy give a quick burst of energy since it is processed faster, which enables the glucose to reach the bloodstream almost immediately. The recommended dietary guidelines recommend that carbohydrates should provide forty-five to sixty-five percent of daily calorie intake. This guideline fluctuates relying on age, gender and activity level (Dietary Guidelines For Americans 2015-2018).
Fats play an important role in cell function within the body and are essential in the structure of steroid hormones. The most widely recognized fats are saturated fats, unsaturated fats, and trans fats. Saturated fats can be found in a variety of foods including, animal meats (beef, poultry, pork), certain plant oils (palm kernel and coconut oil), dairy products (cheese, butter, milk), processed meats (bologna, sausages, hot dogs and bacon), pre-packaged snacks (crackers, chips, cookies, and pastries). In any case, an excess of saturated fats in the blood causes narrowing in the arteries, which could prompt blocked or clogged arteries and increase your risk of heart attack or stroke (Grodner, M.D; 2019 p.76). Saturated fats directly raise cholesterol levels and cause weight gain; by replacing some of your saturated fats with unsaturated fats will help lower LDL cholesterol levels. Common cooking oils, for example, palm oil and coconut oil are very high in saturated fat. Opting for a more advantageous form, for example, monounsaturated fat like olive oil is more beneficial than saturated fats. Other healthy fats include, nuts, fatty fish, plant oils, and avocados (Grodner, M.D; 2019 p.81).
Trans fat consumption appears to increase the risk for CVD. A risk is increased in the light of the fact that the trans-fat raises the blood cholesterol segment LDLs that conveys cholesterol all through the body and, at the same time, may contribute to plaque formation in arteries. Trans fat also decreases the blood cholesterol component (high-density lipoproteins [HDLs]) that removes excess and utilized cholesterol from the body. Maintaining higher levels of this component decreases the risk of CVD. Considering these effects on blood cholesterol, total consumption of trans fatty acids formed from partially hydrogenated oils or naturally occurring in ruminant animal foods should be limited (Grodner, M.D; 2019, p.84). Laws restricting the use of artificial trans fats in the preparation of foods for direct consumption by consumers in restaurants and other food outlets have been implemented in several cities in the United States. The U.S. Food and Drug Administration (FDA) recently proposed removing artificial trans-fat from the Generally Recognized As Safe (GRAS) list of ingredients because of its effect on blood cholesterol levels. The utilization of trans fat would be as a nourishment added substance requiring specific regulations to take into count its utilization (Grodner, M.D; 2019, p.84).
In epidemiological trials, consuming more protein has been recognized to lower blood pressure over some time. Through additional analysis the best source of protein is from plant sources rather than animal sources. From the large cohorts that was involved in this study they suggest that “increased protein intake is associated with reduced risk of ischemic heart disease and perhaps intraparenchymal hemorrhage” (Appel,2003). In different reports a higher protein admission is one characteristic of a dietary pattern associated with reduced risk of ischemic heart disease. The means by which protein could apply it advantageous impacts and incorporate an expanded admission of naturally active amino acids, peptides or highly correlated nutrients (Appel, 2003).
Whey protein, one of the fundamental proteins in milk, may modestly lower blood pressure, according to a small report in the December 2016 American Journal of Clinical Nutrition. Whey is the fluid that is left over after milk and is curdled and strained to make cheese. Evaporating this fluid makes whey protein powder, a supplement popular among athletes and weight lifters for building muscle mass (despite insufficient evidence for this claim). For the study, analyst selected forty-two volunteers with marginally elevated blood pressure. The participants drank two shakes per day that contained whey, casein- another milk protein, or maltodextrin, a carbohydrate that served as a control. They all consumed each of the three supplements for eight weeks each, in random order. Thirty-eight people completed the entire study. In result, consuming fifty-six grams per day of whey protein prompted around a three-point drop in systolic blood pressure and a two-point drop in diastolic blood pressure compared with the control. Both whey and casein additionally prompted better blood vessel function and small improvements in cholesterol levels (Harvard Health Publishing).
Role of Vitamins and Minerals to Hypertension
Lack of certain vitamins and minerals could be a factor for people with hypertension. For example, the mineral potassium plays an important role for heart and muscle function. Some individuals lack potassium in their diet and this is called hypokalemia. Deficiency of this mineral has been linked to hypertension. Unfortunately, certain medications deplete the potassium through urine and by eating fresh fruit and vegetables such as bananas, potatoes, cantaloupe, grapefruit, oranges and prunes is one way of replenishing potassium back into your system. For adults the RDA for potassium is 2000mg (Joy T; 2017 14, August).
Magnesium is another important mineral for the body.” It helps maintain normal nerve and muscle function, support a healthy immune system, keeps the heart beat steady, and help bones remain strong. It also helps regulate blood glucose levels and aid in the production of energy protein” (Magnesium in Diet). In clinical trials it has shown that magnesium lowers blood pressure. With lifestyle change and dietary preventatives the need for antihypertensive medications can be avoided. Diets rich in protein, calcium or vitamin D will increase the need for magnesium. Many dark leafy greens, legumes, milk, soy products and whole grains are rich in magnesium. The RDA for magnesium depends on age and gender (Magnesium in Diet).
It is important to make sure we consume enough calcium in our diet. The right amount of calcium is needed to regulate blood pressure. “The National Institute of Health’s Office of Dietary Supplements credits calcium for proper expansion and contraction of blood vessels, transmitting nervous system impulses and secreting hormones” (Joy T; 2017 14, August). The RDA recommendation for calcium intake is 1000 to 1200mg much of the calcium can be found in dark leafy greens and dairy products (Joy T; 2017 14, August).
Dietary Guidelines and Nutritional Interventions
Lifestyle adjustments with nourishing mediations can prevent or treat hypertension without relying on the use of medications. The 2015-2020 Dietary Guidelines provides five overarching guidelines to inspire people to engage in a healthier lifestyle. As per the USDA, MyPlate delineates the five building blocks of a solid eating regimen using a familiar picture, a place setting. MyPlate centers around utilizing the five food groups to ensure the individual gets the sustenance that they require. With respect to any lifestyle change, this arrangement is customized to the individual to guarantee their objectives are viable and achievable for long-term effect (Dietary Guidelines for Americans 2015-2020).
To begin accomplishing these objectives the first set of guidelines proposes individuals follow a healthy eating pattern across their lifespan. By following and adhering to a good eating pattern people can incorporate the foods they enjoy. It can work for anyone accommodating tradition, culture, and budget. The second guideline centers around variety, nutrient density and amount. This implies individuals need to attempt and keep the calories within normal limits. Choose nutrient-dense foods from all food groups, for example, dark leafy greens, whole fruits, whole grains, lean proteins and low-fat or nonfat dairy. The third guideline states to limit calories from added sugars and saturated fats and reduce sodium (Dietary Guidelines for Americans 2015-2020).
For individuals with hypertension and for people fourteen years and older, MyPlate recommends using no more than 2300mg of sodium, one teaspoon per day. The fourth guideline is to shift to healthy food and beverage choices, for example, instead of sugary drinks, switch to water or consuming full-fat cheese to low-fat cheese. Finally, the fifth guideline is to support healthy eating patterns for all. Encircle yourself with individuals who will bolster your new way of life and urge you to eat better. For a person who is experiencing hypertension, following these guidelines and making the appropriate nutritional changes and physical changes will enhance general well-being and prevent diseases and enable them to live a longer life (Dietary Guidelines for Americans 2015-2020).
Evidence Based Diet Interventions
Dietary Approaches to Stop Hypertension (DASH diet) and the Mediterranean diet are recommendations for individuals who suffer from hypertension. The Dash diet was developed by the U.S National Institutes of Health. This plan was originally implemented to reduce blood pressure. After many studies, it has shown to reduce many diseases like stroke and heart failure. This plan focuses on reducing sodium intake and incorporating more fruits and vegetables into the diet along with low-fat or non-fat dairy and by also including nuts, seeds and beans. This diet plan also focuses on foods high in potassium, calcium and magnesium as well as fiber and protein. As with any lifestyle change you want to make gradual changes. Such as, gradually adding more fruits and vegetables to meals, get added nutrients by including B-vitamin enriched foods as whole grains, such as, whole wheat bread or whole wheat cereal and limited the amount of meat consumed in a week. This plan was not originally used as a weight loss plan, but by following these eating patterns people have also been able to lose weight and decrease high blood pressure within two weeks (Bazzano, L. A., Green, T., Harrison, T. N., & Reynolds, K. 2013, December)
The Dash diet is a successful tool for individuals who are hypertensive because it also focuses on ways to reduce sodium consumption. According to the World Health Association (WHO) the recommendation for salt is two grams per day, less than one teaspoon. The excessive amount of sodium in a person’s diet affects the kidneys by working too hard. The more sodium consumed the more water your body is holding and results in high blood pressure (Why salt is bad). As previously stated, reducing sodium retention is important to take control of high blood pressure. Start out by gradually reducing sodium intake to one teaspoon per day. Once the body has adjusted to the change, then take the next step and reduce taking in sodium to two-thirds of a teaspoon per day. Another way to lower sodium digestion is to read labels and purchase products with low sodium. It is important to know with many processed foods, there are hidden salts added for preservation and taste. Ingredients to watch for are baking soda, soy sauce, monosodium glutamate (MSG), seasoned salt, and antacids. Finding alternative ways to cook with less salt is important, for example, using fresh or dried herb in place of salt. Some individuals use salt substitutes, but these substitutes contain potassium chloride and can be harmful to those who have medical conditions. Other alternatives are buying fresh, frozen or canned vegetables. Take note if buying canned products such as vegetables or tuna it is best to drain and rinse the product to remove any excess sodium. By including calcium-fortified foods, proteins, whole grains and other high- nutrient foods, the Dash diet promotes bone-health and other health outcomes that prevents other diseases like osteoporosis, cancer, heart disease, stroke and diabetes (Is the Mediterranean or DASH Diet Healthier? 2016, May 05).
The Mediterranean diet is another recommended dietary plan to prevent or control hypertension. Although the Mediterranean diet and the Dash diet have similarities, they both recommend increasing the consumption of fruits and vegetables, low-fat or non-fat dairy, fish, and both limit the consumption of red meats. Notably, this diet is based on the traditional foods from the countries that surround the Mediterranean Sea. These people are known to be healthier with lower risks of diseases compared to Americans. The differences the Mediterranean’s use is high intakes of good fats like olive oil, which is the authenticity of the Mediterranean diet, rather than no fat and the allowance of drinking a glass of red wine with a meal. Olive oil is known to provide monounsaturated fats, which help reduce bad cholesterol. Replacement of saturated fats with monounsaturated lipids is associated with the reduction of cardiovascular diseases by reducing LDL cholesterol and promoting HDL cholesterol (T., A., T., D., T., & A.; 2004, October 01).
Additionally, the health benefits of red wine, in moderation, has been known to reduce the risk of heart disease. Red wine has antioxidants called polyphenols, which help protect the lining of the blood vessels in the heart and may increase levels of HDL (good cholesterol) and protect against plaque build-up. Resveratrol, another name for polyphenols, might be the key ingredient in red wine that prevents damage to the blood vessels. Resveratrol is found in the skin of grapes used to make wine (Red Wine and Your Heart; 2016, November 12). Eating grapes or drinking grape is another way of consuming resveratrol without drinking alcohol. Other foods that include resveratrol is peanuts, blueberries, and cranberries. Various research has indicated that all types of alcohol have had heart health benefits, not just wine. It’s thought that alcohol raises HDL cholesterol, reduces the formation of blood clots, helps prevent artery damage associated with too much LDL cholesterol, and may improve the function of the layer cells that line your blood vessels (Red Wine and Your Heart; 2016, November 12). Even though there may be some health benefits of consuming alcohol this must also be done in moderation.
The use of whole grains and brown rice is very common in Mediterranean dishes. It is said that the result of consuming brown rice is more satiating because it takes longer to break down. The slower the digestion the better the nutrients are absorbed and do not create a sugar spike like white rice (Health Studies). The Mediterranean diet is basically plant-based foods, however, consuming fish and seafood twice a week is recommended. As with all diet plans, physical activity is also recommended (Mediterranean Diet 101). By comparison, both diets are highly recommended, and it depends on the eating style of the individual to choose which diet better fits their lifestyle.
Patient education
Nurses are the key role in the start of patients’ wellness. While the patient is in the hospital the nurse is the main person taking part in their care; from the time they are admitted to the time they are discharged. Patient education is vital for successful healing. Patient education first starts with nurses talking to their patients and hearing any concerns regarding their illness and or their treatment. Then set time aside to thoroughly explain to the patient and caregiver about what to expect and what to do after being discharged from the hospital. If the patient needs added support, it is the nurse’s job to produce information of support groups or other professional help. They are responsible for making sure the patient understands the information given to ensure their safety when they are at home.
Regarding individuals who are hypertensive, good nutrition is the platform for overall wellness. Providing diet information such as MyPlate, the Dash diet, and the Mediterranean diet are important to learn because they can be used as the foundation for healthier eating patterns. It is the healthcare professionals’ responsibilities to be knowledgeable of the information before educating patients on their diet regimen. To help patients understand the information they are receiving, healthcare professionals can use interactive education videos and create customized playlists for every patient. This uses all learning styles such as visual, audible, and kinetic learning. Other visual tools can be used such as brochures, models or props, YouTube videos and more. The take away for people who have high blood pressure by incorporating healthier eating habits and changing lifestyle habits hypertension can be controlled and or prevented.
Conclusion
To avoid being a statistic of the one out of three Americans who have hypertension it is crucial to get your blood pressure under control. Controllable risk factors as being overweight, sedentary, consuming foods high in fats and sodium can all be changed by making gradual nutritional and lifestyle changes. Applying nutritional interventions such as using plans like the Dash diet or the Mediterranean diet can prevent or treat hypertension. These plans are both highly recommended by healthcare professionals and these diets have both been proven through studies to lower blood pressure when followed properly.
Reference
An Overview of High Blood Pressure Treatment. (n.d.). Retrieved July 11, 2018, from
https://www.webmd.com/hypertension-high-blood-pressure/guide/hypertension-
treatment-overview
Appel, L. J. (2003, February). The effects of protein intake on blood pressure and cardiovascular
disease. Retrieved July 15, 2018, from https://www.ncbi.nlm.nih.gov/pubmed/12544662
Baker, T. (2016, May 26). So What’s the Deal with Salt? Retrieved August 5, 2018, from
https://ingredientsforchange.com.au/whats-deal-salt/
Bazzano, L. A., Green, T., Harrison, T. N., & Reynolds, K. (2013, December). Retrieved May
28, 2018, from https://www.ncbi.nlm.nih.gov/pmc/articles/PMC4366416/
Diagnosing High Blood Pressure. (n.d.). Retrieved June 25, 2018, from
Dietary Guidelines for Americans 2015–2020 8th Edition. (n.d.). Retrieved May 28, 2018, from
https://health.gov/dietaryguidelines/2015/guidelines/.
Fatty foods. (n.d.). Retrieved July 12, 2018, from
http://www.bloodpressureuk.org/microsites/AfricanCaribbean/Home/Healthyeating/Fattyfoods
Franklin, N. C. (2012, August 27). The DASH Pyramid. Retrieved from
http://ninacheriefranklin.com/you-your-body-and-your-health/the-dash-pyramid/
GRODNER, M. D. (2019). NUTRITIONAL FOUNDATIONS AND CLINICAL APPLICATIONS:
A nursing approach. S.l.: MOSBY.
Harvard Health Publishing. (n.d.). Milk protein may lower blood pressure – Harvard Health.
Retrieved July 15, 2018, from https://www.health.harvard.edu/blood-pressure/milk-1protein-may-lower-blood-pressure
Health Studies. (n.d.). Retrieved June 9, 2018, from https://oldwayspt.org/health-studies?page=2
https://www.medicalnewstoday.com/articles/282929.php
High Blood Pressure. (2018, May 03). Retrieved May 28, 2018, from
https://www.cdc.gov/bloodpressure/index.htm
High Blood Pressure Affects Digestion. (n.d.). Retrieved June 7, 2018, from http://www.
yourhealthdetective.com/2013/05/high-blood-pressure-affects-digestion.html
High Blood Pressure and African Americans. (n.d.). Retrieved June 7, 2018, from
High blood pressure dangers: Hypertension’s effects on your body. (2016, November 23).
Retrieved July 29, 2018, from https://www.mayoclinic.org/diseases-conditions/high-blood-pressure/in-depth/high-blood-pressure/art-20045868
Hypertension? Retrieved June 25, 2018, from https://www.ncbi.nlm.nih.gov/pubmed/27160520
Joy, T. (2017, August 14). What Mineral Deficiency Causes High Blood Pressure? Retrieved
July 31, 2018, from https://www.livestrong.com/article/18749-mineral-deficiency-causes-
high-blood/
Magnesium in diet: MedlinePlus Medical Encyclopedia. (n.d.). Retrieved July 31, 2018, from
https://medlineplus.gov/ency/article/002423.htm
McCance, K. L., & Huether, S. E. (2019). Pathophysiology: The biologic basis for disease in
adults and children. St. Louis, MO: Elsevier.
Mediterranean Diet 101: A Meal Plan and Beginner’s Guide. (n.d.). Retrieved July 1, 2018, from
https://www.healthline.com/nutrition/mediterranean-diet-meal-plan
New ACC/AHA High Blood Pressure Guidelines Lower Definition of Hypertension. (n.d.).
Retrieved July 26, 2018, from https://www.acc.org/latest-in-
cardiology/articles/2017/11/08/11/47/mon-5pm-bp-guideline-aha-2017
Overweight & Obesity. (2018, June 12). Retrieved July 18, 2018, from
https://www.cdc.gov/obesity/data/adult.html
Red Wine and Your Heart. (2016, November 12). Retrieved July 1, 2018, from
https://www.mayoclinic.org/diseases-conditions/heart-disease/in-depth/red-wine/art-
20048281
Symptoms of High Blood Pressure. (n.d.). Retrieved May 28, 2018, from
https://www.webmd.com/hypertension-high-blood-pressure/guide/hypertension-
symptoms-high-blood-pressure
T., A., T., D., T., & A. (2004, October 01). Olive oil, the Mediterranean diet, and arterial blood
pressure: The Greek European Prospective Investigation into Cancer and Nutrition
(EPIC) study The American Journal of Clinical Nutrition | Oxford Academic. Retrieved
July 1, 2018 from https://academic.oup.com/ajcn/article/80/4/1012/4690349
Thibodeau, G. A., & Patton, K. T. (2016). Structure & function of the body. St. Louis, MO:
Elsevier.
What is High Blood Pressure? (n.d.). Retrieved May 28, 2018, from
http://www.heart.org/HEARTORG/Conditions/HighBloodPressure/AboutHighBloodPres
sure/What-is-High-Blood-Pressure_UCM_301759_Article.jsp
Why salt is bad. (n.d.). Retrieved June 7, 2018, from
http://www.bloodpressureuk.org/microsites/salt/Home/Whysaltisbad
Zhu, Z., Xiong, S., & Liu, D. (n.d.). The Gastrointestinal Tract: An Initial Organ of Metabolic
Tables and Figures
Figure 1
Mediterranean Diet Pyramid

Mediterranean Diet. (n.d.). Retrieved August 5, 2018, from
https://oldwayspt.org/traditional-diets/mediterranean-diet
Figure 2
Dash Diet Pyramid

Franklin, N. C. (2012, August 27). The DASH Pyramid. Retrieved from
http://ninacheriefranklin.com/you-your-body-and-your-health/the-dash-pyramid/
Figure 3
Recommendation for sodium intake
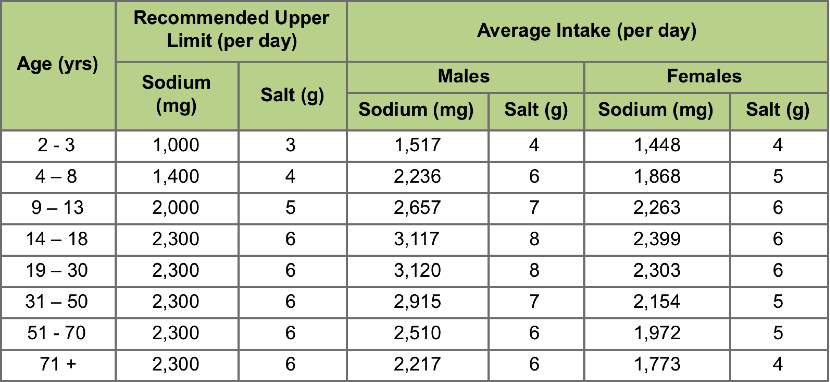
Baker, T. (2016, May 26). So What’s the Deal with Salt? Retrieved August 5, 2018, from
https://ingredientsforchange.com.au/whats-deal-salt/
Cite This Work
To export a reference to this article please select a referencing stye below:
Related Services
View allRelated Content
All TagsContent relating to: "Medicine"
The area of Medicine focuses on the healing of patients, including diagnosing and treating them, as well as the prevention of disease. Medicine is an essential science, looking to combat health issues and improve overall well-being.
Related Articles
DMCA / Removal Request
If you are the original writer of this dissertation and no longer wish to have your work published on the UKDiss.com website then please:




