Medical Plan for Rainforest Expedition
Info: 6093 words (24 pages) Dissertation
Published: 16th Dec 2019
Tagged: Medicine
Living at the extremes
An expedition in the Amazon Rainforest – Matses National reserve; fundraising for the Juvenile Diabetes Research Foundation UK (JDRF).
Type 1 diabetes mellitus accounts for 5-10% of all cases of diabetes mellitus worldwide (Maahs et al., 2010). Medical and technological advancements in the past century, have led to an excellent understanding of the underlining genetics and biological mechanisms. Rigorous research, facilitated targeted and highly effective treatments which imitate defective pathological mechanisms.
The following article attempts to provide a detailed medical plan for a 14-day/13-night expedition, deep into the Peruvian rainforest in November 2018 (01 to 14 of Nov.). The team consists of 7 members: 4 explorers with type 1 diabetes mellitus, an expedition Medic, a local helmsman and a local guide.
The expedition team will venture deep into the Peruvian Rainforest (Amazonia), covering a distance of approximately 110 km, and reside with one of the Amazon’s indigenous tribes, the Matses, at two different locations in the Matses National Reserve in Peru. Additionally, the members will have the opportunity to indulge in once-in-a-lifetime activities like bird-watching, hunting, harvesting, night excursions with motorboats and spotting endemic mammals, anacondas, caimans and pink dolphins.
The team’s ultimate goal is to raise funds for the JDRF UK and disprove misconceptions about the life-limiting nature of the disease. One of the expedition members will be assigned to keep detailed footnotes of the adventure and distribute the experience to the UK media. Following the expedition, the JDRF will sponsor fundraising events in multiple NHS Trust sites, as an opportunity to increase awareness of T1DM and inform the public about its current research initiatives.
This article takes into account the special medical needs of the team and outlines how they will be effectively accommodated in the Peruvian Jungle environment. The first part of the article, presents the intrinsic hazards of the Amazonian jungle, in terms of extreme climatological phenomena, cultural differences, wildlife and endemic diseases whilst addressing prevention measures. The second, addresses the impact of those risks on the explorer with T1DM and suggests clear steps for prevention. The final part, outlines the management plan of critical incidences at the scene.
The expedition itinerary
The full itinerary will be sent to the members by the expedition agency and will include details about the attractions of the expedition. For the medical planning, the timeline of the expedition is presented below, to allow for the quantification of the total exercise per day and possible locations, in case of an emergency:
Day 1 London Heathrow to Lima. Lima to Iquitos.
Day 2 Iquitos to Angamon Village. Motorboat to the first indigenous community.
Day 3 Living with the Matses tribe.
Day 4 Trekking, 20 km North East; camping.
Day 5 Trekking 10km North East; camping near Angamon Village.
Day 6 Trekking 15 km South West; camping.
Day 7 Trekking 15 km South West; camping.
Day 8 Trekking 15 km South West; camping.
Day 9 Trekking 15 km South West; camping.
Day 10 Trekking 15 km South West; reaching the second indigenous community.
Day 11 Living with Matses tribe, location 2; Day 1.
Day 12. Living with Matses tribe, location 2; Day 2.
Day 13 Trekking 5 km to the motorboat. Motorboat to Angamon Village.
Day 14 Iquitos to Lima. Lima to London.
The Amazon; origins and biodiversity
The Amazon river flows across a distance of about 6400 km and is the largest river in the world, in terms of overall water drainage; one fifth of the total water that runs off the continents and into the oceans, is carried by the Amazon river (Alarich R. et al, 2017). In the northeast border of Peru, the Ucayali River merges with the Mantaro river to form the main stream of the Amazon river. The region owes its biodiversity, thick plantation and immense rainforests (Amazonia) to the vast Amazon basin and the huge water volumes it carries out to the mouth of the Atlantic Ocean in East Brazil. The fauna of the region if famous for: a variety of endemic birds and fish species, mammals including sloth bears, pumas, monkeys and reptiles like anacondas and caimans. The flora is equally diverse. The region offers an opportunity to find trees that reach up to 40m. height (Rainforest Conservation Fund, 2017) and plants from which licenced phytomedicines like quinine derive.
The Matses tribe
The Matses tribe is an indigenous rainforest tribe with a population of approximately 2200 people, who made their first contact with the rest of the world in 1969.
Their survival mainly relies on the rainforest itself, with very few goods imported. Harvesting, gathering and hunting with arrows and bows, are the main sources of food. Few individuals engage in minor commercial activities like trading meat.
From a spiritual point of view, Matses believe there is a spirit in every form of life. There are certain taboos around which animals they are allowed to hunt, and certain rituals on how to use tree produces (Wikipedia, 2018)
Matses are peaceful and used to visitors. To be accepted by their community and establish trust, explorers are advised to visit escorted by local guides.
Matses National Reserve, Requena Province, Peru; climate and risks
The area of Requena, Peru has tropical rainforest climate, according to Köppen climate classification system (McKnight and Hess, 2000).
The mean temperature reaches 32 °C in the daytime and drops to 22 °C in the night-time. This accounts for a significant temperature decrease within a day. Humidity in November can be as high as 95%, and winds are mild, with the mean wind speed registering at 3.5 mph (World Weather Online, 2018). The combination of high temperature, humidity and rare winds, along with the necessity of full body coverage with clothes to prevent insect bites, facilitate fast dehydration in travellers pursuing outdoor physical activities. On the other hand, quickly decreasing temperatures in the night require warm clothing.
Furthermore, rainfalls are heavy and frequent throughout the year in the Peruvian rainforest. However, the rain is more pronounced during the wet season (November to April). The average rainfall in November comes roughly up to 256mm (The only Peru Guide, 2018). To better comprehend these figures, it is worth comparing them with rainfall in London. November in Requena, a month of moderate rainfall for the region, has 360% more rainfall than October in London, the wettest month of the year.
Despite the high UV index of six (WHO’s Global UV Project, 2002), thick vegetation creates plenty of natural shade whilst trekking in the rainforest. Nevertheless, harm from sun can still be high, and travellers who use motorboats to reach remote forest areas need to be fully protected with adequate white, long-sleeved tops and trousers, as well as, hats and sunglasses (World Weather Online, 2018).
In the region, water levels can rise up to 7m in the wet season, rapidly expanding the surrounding flood plains and determinedly changing the geography of the area (Yr – Weather statistics, 2018). Campers should be prepared to quickly adjust their plans and turn to drier locations, in view of these remarkable effects of the rain. Water currents can be fierce, and expedition teams traveling by boats should have handy evacuation plans at all times. Hiring a safe boat and choosing a reliable travel agency are paramount to avoid disasters. Equipment preservation, food supplies and clothing can also be affected by heavy rain thus posing the risk of sudden termination of the expedition. Last but not least, rain turns hectares of flat land into swamped islands, attracting a diversity of disease carrying vectors, like mosquitos.
 Matses National Reserve, Requena Province, Peru; wildlife and risks
Matses National Reserve, Requena Province, Peru; wildlife and risks
Mammals, like puma and jaguar are common throughout the region, but unlike common belief, they avoid contact with humans unless provoked. Other endemic mammals, like monkeys and bats can also transmit zoonosis like rabies. To avoid disasters, it is advisable to be wary of those direct and indirect dangers and follow the advice of the local guides; many of them used to be hunters in the rainforest and can easily identify danger and respond.
The Amazonia also harbours a variety of snakes: the pit vipers (Fig. 1) are venomous and the amazon boas, although non-venomous, can cause death by suffocation. Other venomous animals in the region are the bullet ants, the Amazonian centipede, the assassin bug and the poison dart frog (Fig. 2) (IP factly, 2015). Before visiting the area, explorers should be educated in recognising dangerous species and avoiding contact.
Figure 1: Pit Viper (IP factly, 2015)
As a general rule, boots should be carefully shaken and inspected to
identify any tears that might give access to insects and water.
 Finally, swimming in the Amazon can be risky too. Electric eels and
Finally, swimming in the Amazon can be risky too. Electric eels and
piranhas, although rarely fatal, can cause severe nuisance, if they attack humans in remote areas (IP factly, 2015).
Amazonia in Peru; endemic diseases
Prevention
In the Amazonian Peru, many preventable diseases are endemic. The majority of them are mosquito-borne, like the yellow fever, dengue and malaria. Initial symptoms are non-specific and involve headache, fever, malaise, myalgia and loss of appetite. Tick bites can also transmit diseases, like Lyme disease; general protection measures offer prevention:
- Long-sleeved tops
- Full length trousers, treated with permethrin
- Closed toe shoes/boots
- Mosquito nets
- DEET 30% repellents applied every 6 hours as a minimum; depending on activity. DEET can decrease the sunscreen protection thus sunscreen should be applied more frequently when DEET is co-applied (Public Health England, 2013) (CDC, 2017).
Additionally, UK health services have announced that Peru is at risk of having Zika virus. As this is a mosquito-borne disease, (cases of sexual transmission have also been reported), the rules above apply for the prevention of this disease too (GOV.UK, 2018).
Vaccines
The following vaccinations are strongly recommended by the UK Health Services:
- Routine vaccinations
- Yellow fever
- Typhoid
- Hepatitis A
- Rabies
- Tetanus-containing vaccine/booster
(Health Travel Pro, 2018)
Chemoprophylaxis
The risk of malaria in the region is high. Malaria prophylaxis tablets should be prescribed and administered as follows:
- Atovaquone/Proguanil 250 mg/100mg film-coated tablets (Malarone tablets), one tablet daily. Prophylaxis commences 2 days before travelling to Peru and 7 days after returning to the UK.
Note: Chloroquine tablets is the first line prophylaxis. Due to risk of hypoglycaemia in individuals with diabetes mellitus, Malarone tablets are recommended as an alternative.
(Public Health England, 2013)
Other preventive measures:
The team will be exposed to different hygiene standards when living in the jungle. For this matter, several other issues should be also addressed. Food conditioning and preparation within the tribe can be very risky. Viruses, bacteria/toxins and parasites can cause gastrointestinal disorders, ranging from simple traveller’s diarrhoea to more severe haemorrhagic versions. Moreover, serious infectious diseases can be transmitted by ingestion of raw meat, like brucellosis. For all the aforementioned reasons, team members should comply with these guidelines for hygiene-keeping:
- Thorough sanitisation of hands after handling raw meat, raw vegetables, before eating, before and after toileting. Soap and hand hygiene gels are recommended.
- Toileting 50m away from accommodation/river. Wipes and hygiene pads should be kept in the rubbish area.
- When camping by the river, there will be 3 agreed ‘river zones’ according to the water flow: upper zone for potable water, middle zone for dish washing, lower zone for toileting.
Above recommendations are essential for participating in the expedition. The participants are strongly advised to visit their General Practitioner 6 weeks prior to departure and provide evidence that their vaccination status is up-to-dated and chemoprophylaxis has been initiated.
Other expedition-specific health risks
Preventing hypoglycaemia and hyperglycaemia:
Exercising in hot climate, on one hand increases caloric consumption and on the other exacerbates water and electrolyte loses.
As indicated in the adventure’s itinerary, the team is planned to trek a distance of approximately 110km within 8 days. The maximum kilometres per day are 20km and the minimum 5km. The trekking speed will be 2.5km per hour thus the maximum trekking duration will be 8hrs/day. Trekking at this pace corresponds to exercise intensity of 3 METS (WHO, 2014). Simple calculations using the following formula: 1 MET = 3.5 ml O2/kg/min or approximately 1 kcal/kg/hour (Wikipedia, 2017), result in consumption between 1200 kcal to 1920 kcal, for 8 hrs of trekking (these calculations are based on the members’ weight and do not include extra caloric consumption due to body thermoregulatory mechanisms (Michael N. Sawka et al, 1993) and carried load). This amount of exercise will increase the overall daily requirements for a person weighting 80kg to 3840kcal in total, assuming that activity levels will drop to 1-2 METS for the rest of the day.
The expedition is planned to accommodate the dietary needs of its participants. Five meals are scheduled for each day. The meals will include rice (white), quinoa, fruits (passion fruit, mango, papayas, banana), nuts, vegetables (roots, plantains) and fish (Paley, 2014). Meat will also be available. It might come from reptiles, turtles, snakes, caiman and chicken (Staff writer, 2018).
Meals will be served with the tribe on the 2nd, 3rd ,11th and 12th night. Extra supplies of rice, quinoa, potatoes, onions, tomatoes, bananas, sunflower oil, canned tuna, dark chocolate, spaghetti, bread slices, cheese slices will be stocked in the motorboat (total of 67.2kg for food supplies: 1.2kg per person per day x 8 days x 7 individuals). The team will be trekking with the motorboat at a reachable distance of 5km at all times. A sample of careful meal planning for a 3hr trek is given below:
- 5 meals per day, calculated according to maintenance and exercise caloric requirements: Breakfast: 2 bananas plus 4 biscuits (200gr, 474 kcal), brunch: sandwich with cheese + `(optional) 4 biscuits (170gr, 602 kcal), lunch: whole-wheat spaghetti with tuna (195g, 560kcal), evening: rice (200g, 262 kcal) with tinned beans (150 gr, 121kcal) and dark chocolate (100gr, 507 kcal), sandwich with cheese (70g, 328kcal) plus 1 banana (100gr, 95 kcal) plus (optional) dark chocolate (100g, 507kcal). Total calories: 2675kcal – 3456kcal. Total weight: 1185g-1285g per day.
(NHS Choices, 2016)
Recognising hypoglycaemia:
Prompt recognition of hypoglycaemia and self-awareness, save valuable time and can prevent disasters. The members of the team are likely to have already experienced relevant symptoms and the topic will be presented in the pre-departure meeting though a simple interactive teaching session.
Medical management of hypoglycaemia in the scene (adapted from NICE guidelines)
- For alert patients glucogel will be given orally.
- For unresponsive patients, intramuscular glucagon will be administered.
- According to response, decision for evacuation will be made by the medic.
(BNF: British National Formulary, 2017a)
The author strongly recommends:
- Carrying glucometers at all times, testing strips and lancets (and sufficient supplies for each).
- Carrying solar calculators and adjust your rapid and long acting insulin dose according to above estimations.
Preventing dehydration, electrolyte imbalance:
Water and salt/electrolyte losses are difficult to quantify. Miller and Bates, attempted to calculate salt losses in individuals working at their 40% VO2 max, for 8-12 hrs, in 30°C -35°C. According to their results sodium losses were 4.8g to 6g and the average water loss 7.8ml/min (Bates and Miller, 2008).
Critically considering those results, the author recommends:
- The use of dioralyte supplements (Dioralyte Natural/Citrus/Blackcurrant, 3.5g/470mg/300mg/530mg), four times per day (7 days x 4 sachets/day = 28 sachets).
- Consumption of at least 3L of water (for losses) plus 2.7L for females/3.7L for males (for maintenance) per day.
Above recommendations apply for the days of long trekking and specific information based on the trekking schedule and individual needs, will be provided in the pre-departure briefing meeting.
Preventing heat stroke and dehydration:
There is abundance of water from the river and different purifying methods will be available. The team will trek in close proximity to the river, to ensure easy access to water. The author recommends:
- Light, loose and long-sleeved white clothes.
- Wide-brimmed hats.
- Water consumption with dioralyte supplements, as highlighted above.
- Consuming adequate water volumes at all times, in a scheduled way. Hourly breaks for water will take place during trekking and with meals.
Medical management of dehydration in the scene
- Intravenous fluids will be available for rigorous hydration in extreme circumstances. The victim will be evacuated as a major incidence (see ‘evacuation’ section).
Diabetic Ketoacidosis; Medical management in the scene
- IV fluids, enhanced with potassium will be stored in the boat’s refrigerator. In case of suspected diabetic ketoacidosis, the treatment will commence in the scene but only as an intermediate measure until transfer to the hospital. The victim will be evacuated as ‘a major incidence’ (see ‘evacuation’ section).
(BNF: British National Formulary, 2017b)
Foot wounds/Minor injuries
Foot wound and minor injuries are very likely to happen due to hiking in humid environment. The author recommends:
- Foot inspection and hygiene will be a priority every morning.
- First aid kit for minor injuries will be available.
Fractures
Reduction and immobilisation of fractures will happen in the scene.The victim will be evacuated as ‘a minor incidence’ (see ‘evacuation’ section), unless signs of neurovascular compromise.
Managing T1DM in the Peruvian Jungle
Insulin can last for up to a month in room temperature. A refrigerator will be available in the motorboat and individual storing bags are recommended for all participants (Independent Diabetes Trust, 2018). Glucose measurements will follow the same routine as in non-extreme environments for early identification of abnormalities.
Communication
The expedition will carry the appropriate means of communications, both internally between its members and externally, in order to ensure the safety of the participants.
Internal communication devices will include 10 HF radios (“Woki-tokies”), one for each participant and three for contingency. The frequencies calibrated on the devices will include main and reserve internal communication channels, and additional channels for external communications as detailed below. Each participant in the expedition will carry his own device and will be required to charge and check the device’s functionality with the group on a daily basis. While on the boat, HF radios will be switched off except for one, listening to the regional emergency frequency. While trekking, the members at the lead and the tail of the group will switch their devices on the main internal channel, while the other members will keep their devices switched-off for battery saving. Participants who find themselves detached from the group will be briefed to hold their position, switch-on their radios and call on the main group’s frequency (switching to the reserve if no communication is established within 15 minutes).
External communication will rely predominantly on three satellite phones, one present on the boat at all times and two carried by the group. HF radios will be used for external communication as a contingency (mobile phones are considered as a last resort due to poor coverage in the area). In the case of an emergency, the satellite phone will be used for communicating with the search and rescue units listed below (passing the accurate location of the boat along with all medical details). In the case of poor satellite signal, the phone on the boat should be used, as vegetation should be less dense directly above the river.
The following phone numbers and frequencies should be calibrated for speed-dialing on the expedition’s devices:
Search and rescue contacts (Sarcontacts, 2018):
- SRR Peru – +51 1 420 2020
- Iquitos Air Force Base (Base Aérea Coronel Francisco Secada Vignetta IAP) – [Number missing, to be obtained in communication with Iquito international airport]
- Aeronautical emergency frequency – 121.5 MHz (123.1 MHz auxiliary) (ntc.gov, 2016)
Iquitos hospitals:
- Hospital Regional de Loreto “Felipe Santiago Arriola Iglesias” – +51 949 542 444
- Iquitos Hospital Garayar César García – +51 65 263749
The medical kit
The medical kit of this expedition is customised based on the climate, outdoor activities and the special health conditions on the members. An Insulated cooler (10L) and a small refrigerator (5L) will be available on the boat. Each individual will be instructed to carry a maximum of 7kg. Travelling in the jungle with a motorboat, allows for heavy equipment to remain stored in the boat.
Mediations PO/IV/IM:
Analgesics: the available pain killers will be paracetamol and ibuprofen.
Antibiotics: The antibiotic for the treatment of severe diarrhoea is ciprofloxacin with good sensitivities for the area (NICE, 2013). Another useful antibiotic agent is co amoxiclav 625 mg for infected wounds.
Antidiarrheal drugs: Loperamide tablets.
For hypoglycaemia: 1) Glucose 400 mg per 1 gram, 75mg tubes 2) IM glucagon 1mg vials x 4 3) IV fluids: 500 ml of NaCl 0.9% + 20mmol KCL.
Anaphylaxis: 1) IM Adrenaline 300mg (Epipen) 2) Prednisolone 5mg tablets 3) IV/PO chlorphenamine and cetirizine.
Wounds: Irritating skin conditions are common in tropical environments. Fusidic acid 2%, 1% clotrimazole and 1% hydrocortisone will cover the majority of them, together with simple measures of wound care. For minor injuries like abrasions and lacerations, steristrips, glue and sutures will be provided, along with antiseptic spry, roll of zing, bandages and simple dressings.
Severe wounds will require more advanced equipment and possibly evacuation. Fractures will be reduced and splinted with SAM splints and Kendrick Traction Devices, since both have the advantage of being very light and easy to apply (Hudson S., 2018).
Bites: In the event of bites from non-venomous species, the wound management will include thorough irrigation of the area and antibiotic prophylaxis. Although, the local guide is extremely well trained in recognising venomous species, the likelihood cannot be minimised. The Medic will carry at all times, one vial of the European viper snake venom antiserum 20ml vial. This will only delay the effects of the venom in the organism, if combined with careful irrigation of the skin, application of tourniquet and IV fluids. In case of such an emergency, the victim will be immediately evacuated.
Other Equipment: Basic equipment for the measurement of the vital signs, like sphygmomanometer and oximeter will be available. The Medic will also carry one Glucose and ketone meter (+ batteries) as a contingency. Once recognised, the treatment will be initiated at the scene and will be continued in a secondary care environment.
Casualty Evacuation plan: Casevac
Risks are inherent in an expedition. The risk assessment for this expedition, has taken into account the tropical climate of the location, its distance from specialised in-hospital care, the quality of this care and the members’ special needs. Emphasis has been given on several prevention measures for elimination or minimisation of risk. Conditions like hypoglycaemia, dehydration, diabetic ketoacidosis and venomous bites, are priority 1B emergencies which require immediate evacuation after transfer to the river bank.
The expedition itinerary involves trekking for pre-planned distances with a maximum distance of 5km from the river bank. On one hand, this will ensure rapid access to further medical supplies (on the motorboat). On the other, it will facilitate timely transfer to an open-air location (motorboat), from where aerial evacuation is possible.
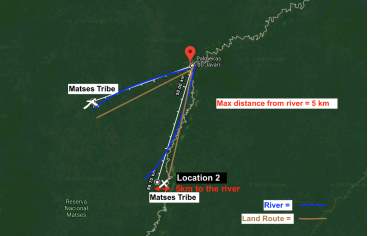 As demonstrated in the map (Fig. 3), the nearest health facility, is a secondary Public Hospital in Iquitos (Hospital Regional De Loreto). The hospital is open 24/7 and accepts emergencies. It can accommodate the needs of severe injuries and acute medical conditions, offer inpatient care and emergency surgeries, X-Rays, blood tests and body scans (‘Hospital Regional de Loreto and Belen Clinic in Iquitos, Peru’, 2018).
As demonstrated in the map (Fig. 3), the nearest health facility, is a secondary Public Hospital in Iquitos (Hospital Regional De Loreto). The hospital is open 24/7 and accepts emergencies. It can accommodate the needs of severe injuries and acute medical conditions, offer inpatient care and emergency surgeries, X-Rays, blood tests and body scans (‘Hospital Regional de Loreto and Belen Clinic in Iquitos, Peru’, 2018).
Figure 3
Casevac:
The farthest point from the boat the team is planned to be during the expedition, is location 2. One of the Matses tribes lives in location 2, right on the border between Peru and Brazil. Location 2 is 50km away from the nearest airport in Angamon and 5km away from the river. A helicopter from the Iquitos Army base, can approach Angamon within 1.5hr and Location 2 within 2 hours (Fig. 4).
When the casualty needs evacuation in the next 12 hrs or more, the preferred plan includes transfer by motorboat to Angamon Village and from there, by air to Iquitos. The total duration of a transfer, in this scenario, is 8.5 hrs: 6 hrs by boat and 2.5 hrs by air. Once on board, the Medic will notify the air force base in Iquitos. Once the boat is dispatched to Angamon, the Medic will contact the Iquitos Hospital, to alert them for the air ambulance’s pending arrival.
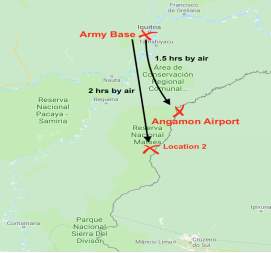 In the case of a priority 1B casualty in location 2, the team will aim to transfer the patient as fast as possible, covering the 5km distance. If time permits, this can be done with stretches made of rope or manually, by the team members (2hrs). The medic will notify the army airbase at the time of the incidence. Once the casualty is in safe position on the boat’s stretcher, the helicopter can approach from above. The helicopter can arrive in the area of location 2 (from Iquitos) within 2 hrs.
In the case of a priority 1B casualty in location 2, the team will aim to transfer the patient as fast as possible, covering the 5km distance. If time permits, this can be done with stretches made of rope or manually, by the team members (2hrs). The medic will notify the army airbase at the time of the incidence. Once the casualty is in safe position on the boat’s stretcher, the helicopter can approach from above. The helicopter can arrive in the area of location 2 (from Iquitos) within 2 hrs.
Figure 4
The Casevac will be presented in the pre-departure meeting to all team members and to the local guide upon arrival, and printed material with all the emergency contacts will be handed out. Team awareness is imperative, for effective team-working and stress management.
It is important to note, that in emergency cases, where the Medic needs to be off-site accompanying a patient, the team should disengage from all high-risk activities. The responsibility at those times, will be handed over to the local guide.
(Operation Wallacea, 2017)
(World Extreme Medicine, 2013)
Other topics:
Member should be aware of country specific regulations regarding identification documents and transportation within the country. The team members should ensure that their passport is valid for 6 months from the day of entry in Peru. On a different note, transportation in Peru is risky due to poor driving standards and increasing incidences of robbery and crime at the bus stations or by taxi drivers. Transportation from and to the airport is planed under a reliable private company which complies with international safety regulations. Transportation in Iquitos with the agency’s private vehicle guarantees comfort and safety (gov.uk, 2018).
Each member should submit a relevant health questionnaire at least 6 weeks before the expedition. The questionnaire needs to be signed by the GP and will include the most up to date prescription and immunisation records.
Conclusion:
Detailed pre-planning lies in the core of successful and rewarding expeditions. In the rainforest, risks mainly arise from the tropical climate and the isolation of the explorers from reliable health services, locally established evacuation systems and endemic diseases. Less apparent risks, like wild animals and unfamiliar codes of contact, can also have devastating effects on the team. Moreover, diabetes itself can exacerbate the effects of dehydration, poor nutrition and intense exercise. The team’s and the Medic’s preparedness are essential and are addressed through prevention measures, robust evacuation planning, fully equipped medical kit and education.
Surviving in tropical environments can pose risks to health and safety, despite thorough risk assessment and safety systems. The question of whether the medical risk in extreme environments, is ever going to be acceptable, is yet to be answered.
References:
- Alarich R. Schultz James J. Parsons Raymond E. Crist (2017) Amazon River, Britannica.com. Available at: https://www.britannica.com/place/Amazon-River.
- Bates, G. P. and Miller, V. S. (2008) ‘Sweat rate and sodium loss during work in the heat.’, Journal of occupational medicine and toxicology (London, England). BioMed Central, 3, p. 4. doi: 10.1186/1745-6673-3-4.
- BNF: British National Formulary (2017a) ‘Diabetic ketoacidosis’, BNF: British National Formulary. NICE.
- BNF: British National Formulary (2017b) ‘Hypoglycaemia’. NICE, 74.
- CDC (2017) Health Information for to Peru Clinician View. Available at: https://wwwnc.cdc.gov/travel/destinations/clinician/none/peru.
- NHS Choice, ‘Calorie counter’, 2016. Department of Health.
- GOV.UK, Entry requirements – Peru travel advice, 2018. Available at: https://www.gov.uk/foreign-travel-advice/peru/entry-requirements.
- health travel pro, health travel pro, 2018. Available at: https://travelhealthpro.org.uk/country/177/peru#Vaccine_recommendations.
- ‘Hospital Regional de Loreto and Belen Clinic in Iquitos, Peru’, 2018.
- Independent Diabetes Trust (2018) Storing Insulin. Available at: https://www.iddt.org/about/living-with-diabetes/storing-insulin.
- IP factly, Top 15 Most Dangerous Animals in the Amazon Rainforest, 2015. Available at: http://ipfactly.com/top-15-dangerous-animals-amazon-rainforest/.
- Maahs, D. M. et al. (2010) ‘Epidemiology of type 1 diabetes.’, Endocrinology and metabolism clinics of North America. NIH Public Access, 39(3), pp. 481–97. doi: 10.1016/j.ecl.2010.05.011.
- McKnight, T. L. (Tom L. and Hess, D. (2000) Physical geography : a landscape appreciation. Prentice Hall.
- Michael N. Sawka,1 C. Bruce Wenger, Andrew J. Young, and K. B. P. (1993) Physiological Responses to Exercise in the Heat, Nutritional Needs in Hot Environments: Applications for Military Personnel in Field Operations. Edited by Marriott BM. National Academies Press (US).
- NICE (2013) ‘Antibiotic treatment for travellers’ diarrhoea’. doi: 10.1002/14651858.CD002242.
- Operation Wallacea (2017) ‘Medical and Evacuation Procedures’.
- Paley, M. (2014) We Are What We Eat: Foraging in the Amazon Rainforest, National Geographic. Available at: https://www.nationalgeographic.com/photography/proof/2014/10/15/we-are-what-we-eat-foraging-in-the-amazon-rainforest/
- Public Health England (2013) ‘Guidelines for malaria prevention in travellers from the UK’, p. 97.
- Rainforest Conservation Fund, General features of tropical plants, 2017. Available at: http://www.rainforestconservation.org/rainforest-primer/rainforest-primer-table-of-contents/e-composition-of-tropical-rainforests/3-general-features-of-tropical-plants/.
- Sean Hudson (2018) What to put in your expedition medical Kit expedition medicine course training, Wold Extreme Medicine. Available at: http://www.expeditionmedicine.co.uk/index.php/advice/resource/r-003.html.
- Sean Hudson, Risk Assessments and Casualty Evacuation, Across the Divide Expeditions & Dr Sean Hudson. Available at: http://www.expeditionmedicine.co.uk/index.php/advice/resource/r-0014.html.
- Staff writer, Peru Food- Amazon | Discover Peru. Available at: http://www.discover-peru.org/peru-food-amazon/.
- The only Peru Guide, Weather in Iquitos and Around. Available at: https://theonlyperuguide.com/peru-guide/amazon-jungle-peru/weather-in-the-amazon-jungle/.
- WHO | What is Moderate-intensity and Vigorous-intensity Physical Activity?’ (2014) WHO. World Health Organization
- Wikipedia, Matsés, 2018. Available at: https://en.wikipedia.org/wiki/Matsés.
- World weather online, Iquitos, Loreto, Peru Weather Averages. Available at: https://www.worldweatheronline.com/iquitos-weather-averages/loreto/pe.aspx).
- Yr – Weather statistics for Pacaya Samiria National Reserve, Loreto (Peru) 2018. Available at: https://www.yr.no/place/Peru/Loreto/Pacaya_Samiria_National_Reserve/statistics.html.
- Global UV Index, WHO’s Global UV Project, 2002. Available at: http://www.who.int/uv/publications/en/UVIGuide.pdf
- Search and rescue contacts, Sarcontacts. Available at: https://sarcontacts.info/srrs/pe_pru/
- National Telecommunications Commission. Available at: http://ntc.gov.ph/wp-content/uploads/2016/nrfat/NRFAT-2016-Rev-2.pdf
- Metabolic Eqiuivaletn, Wikipedia, 2017. Available at: https://en.wikipedia.org/wiki/Metabolic_equivalent
The author: 670059975/2
Cite This Work
To export a reference to this article please select a referencing stye below:
Related Services
View allRelated Content
All TagsContent relating to: "Medicine"
The area of Medicine focuses on the healing of patients, including diagnosing and treating them, as well as the prevention of disease. Medicine is an essential science, looking to combat health issues and improve overall well-being.
Related Articles
DMCA / Removal Request
If you are the original writer of this dissertation and no longer wish to have your work published on the UKDiss.com website then please:




